An open sore, or ulcer, that grows on the foot is one of the most common injuries in persons with diabetes—a condition in which the body has difficulty controlling blood sugar levels. Without management, even a little blister on the foot can quickly turn into an open sore. Diabetes patients sometimes suffer nerve damage known as peripheral neuropathy, which prevents them from feeling foot discomfort, thus any form of a blister, cut, or scrape may go untreated.
Diabetes foot ulcers could be prevented. Daily foot checks ensure that any injury is addressed as soon as possible before it becomes an open sore. Maintaining a healthy weight and managing your blood sugar levels will help your body stay healthy, which can speed up healing.

WHO IS AT RISK OF DEVELOPING A DIABETIC FOOT ULCER?
Diabetes can cause a foot ulcer in anyone. Ulcers are more common in Native Americans, African Americans, Hispanics, and older men. Insulin users, as well as those with diabetes-related kidney, eye, and heart illnesses, are at a higher risk of getting a foot ulcer. Being overweight, as well as using alcohol and smoking, all contribute to the development of foot ulcers.
WHAT CAUSES DIABETIC FOOT ULCERS?
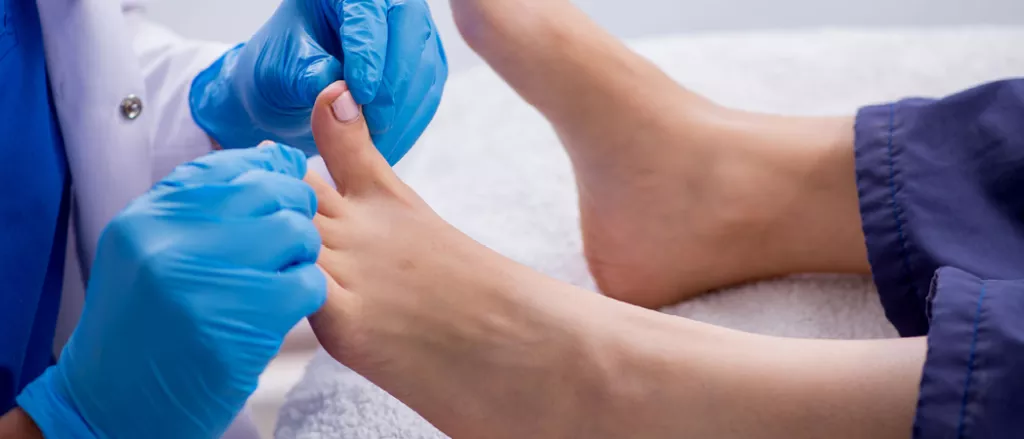
Ulcers arise as a result of a mix of circumstances, including a loss of sensation in the foot, poor circulation, foot abnormalities, irritation (such as friction or pressure), trauma, and the length of diabetes. Patients who have had diabetes for a long time may develop neuropathy, which is characterized by a diminished or complete inability to feel pain in the feet as a result of nerve damage induced by rising blood glucose levels over time. Nerve damage can often occur without pain, and the patient may be unaware of the problem. A simple and painless piece of equipment called a monofilament can be used by your podiatrist to test your feet for neuropathy.
Vascular disease can make a foot ulcer worse by impairing the body’s ability to heal and raising the risk of infection. Elevated blood glucose levels can impair the body’s ability to fight off infection and potentially slow healing.
HOW IS A DIABETIC FOOT ULCER TREATED?
The fundamental goal of foot ulcer treatment is to achieve healing as quickly as feasible. The faster the wound heals, the less likely an infection will occur.
There are numerous vital aspects to consider when treating a diabetic foot ulcer:
- Infection prevention
- Taking the strain off the area is referred to as “off-loading.”
- Debridement is the removal of dead skin and tissue.
- Using medication or dressings to treat the ulcer
- Managing blood glucose levels and other health issues
Not all ulcers are infected; however, if your podiatric physician identifies an infection, you must follow a treatment plan that includes antibiotics, wound care, and maybe hospitalization.
TIPS FOR PREVENTING DIABETIC FOOT ULCERS
Foot care in diabetes patients is unavoidable in the prevention of infection and necrosis, failing which would worsen the situation and leave them with no other option but a diabetic foot ulcer amputation.
- Diabetes Management: Diabetes is a chronic disease that does not go away, whether you are recently diagnosed or have been living with it for years. Dealing with it can be difficult because it becomes your complete job to manage it through your food, exercise, and several other duties several times a day. Your doctor can only give you suggestions and guidelines for managing your blood sugar levels; you must strictly follow the directions to stay healthy. You and your doctor will be able to plan a chart for your routine diabetes care because it is not the same for everyone. Diabetes management may entail food planning, physical activity, and regular blood sugar readings. In addition, one’s emotional response to diabetes, stress levels, and imbalances all play a role in developing a healthy lifestyle. While the need to evaluate and follow many areas of your daily life may appear complicated, this complexity can be reduced by planning and managing diabetes efficiently.
- Check your feet daily: Diabetics should check both feet regularly for blisters, scrapes, scratches, and ingrown toenails. It’s also a good idea to check the bottom of each foot using a mirror, as blisters frequently form there. Doctors also advise keeping an eye on your feet for signs of infection, such as redness, swelling, and warmth. If you experience these changes, seek medical attention right once.
- Proper Footwear: Wearing shoes that do not fit properly increases the likelihood of a blister. Shoes should not be too small, too big, or too small. Because foot size and width can alter over time, doctors advise getting your feet measured anytime you buy new shoes. A properly fitting shoe contains half an inch of space between the toes and the tip of the shoe and offers enough arch support. Podiatrists advise wearing clean, dry socks with no tight elastic bands that may limit blood flow to the foot. Doctors urge diabetics to avoid walking barefoot or wearing sandals, as these expose their feet to splinters, concrete, or sand, which can scrape or irritate the foot. You should also avoid wearing high-heeled shoes since they place too much strain on your feet.
- Weight Loss: Being overweight or obese puts extra strain on the feet, which can cause friction and blisters when wearing shoes. Specialty Care Clinics’ dietitians and nutritionists can assist you in losing weight. If you are unable to control your blood sugar levels due to obesity, you and your doctor can discuss the option of weight loss surgery.
- Diet: Diabetes medicine and wound healing go hand in hand. Diabetes patients should eat food based on its effect on their blood sugar levels. Each type of meal may affect blood sugar differently, and it is critical to be aware of this. As vital as choosing the appropriate type of food is knowing how much to eat.
- Exercise: As crucial as food is for diabetic foot ulcer healing, staying active is equally important since it helps your body use insulin more efficiently. Any physical exertion generates energy from blood sugar. As a result, the more committed you are to staying active with light to moderate exercise, the better your blood sugar control will be.
- Ceasing Tobacco: Cigarettes and other tobacco products include compounds that delay healing, making a full recovery from a foot ulcer unlikely. Tobacco products have also been related to circulatory disorders, including an increased incidence of lower limb artery disease, which lowers blood flow in the legs and feet.
OUTLOOK
People with diabetes not only do not heal as well as non-diabetics, but they also acquire a disorder called diabetic neuropathy, which causes them to lose feeling in their feet.
Our experts at Specialty Care Clinics will take care of your health and help you recover from diabetes and its effect on your feet. Specialty Care Clinics has cutting-edge medical care to diagnose any serious and chronic medical problems. Call us at (469) 545-9983 to book an appointment with our specialists.
