VIRAL GASTROENTERITIS – SYMPTOMS, CAUSES, AND TREATMENT
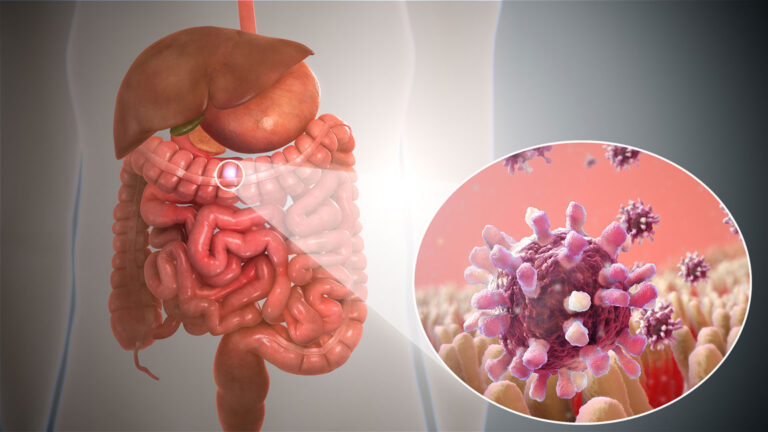
Viral gastroenteritis is an intestinal infection that includes signs and symptoms like watery diarrhea, stomach cramps, nausea or vomiting, and at times fever.
The most common way to develop viral gastroenteritis — often known as stomach flu — is through contact with an infected person or by consuming contaminated food or water. If you are otherwise healthy, you will probably heal without complications. But for infants, older adults, and people with compromised immune systems, viral gastroenteritis could be deadly.

There is no effective treatment to treat viral gastroenteritis, so prevention is the key. Avoid food and water that might be contaminated and wash your hands thoroughly and often.
SYMPTOMS
Although it is commonly known as stomach flu, gastroenteritis is not the same as influenza. The flu (influenza) affects only your respiratory system — your nose, your throat, and your lungs. Gastroenteritis, on the other hand, attacks your intestines, causing signs and symptoms like:
- Watery, usually non-bloody diarrhea — bloody diarrhea generally means you have a different, more severe infection
- Nausea, vomiting, or both
- Stomach cramps and pain
- Occasional muscle aches or headache
- Low-grade fever
Depending on the cause, viral gastroenteritis symptoms might appear within one to three days after you are infected and could range from mild to severe. Symptoms generally last just a day or two, but occasionally they might last up to fourteen days.
Because the symptoms are similar, it is easy to confuse viral diarrhea with diarrhea caused by bacteria, like Clostridioides difficile, salmonella, and Escherichia coli, or parasites, like giardia.
WHEN SHOULD YOU SEE A DOCTOR?
If you are an adult, call your health care provider if:
- You are unable to keep liquids down for 24 hours
- You have been vomiting or having diarrhea for more than two days
- You are vomiting blood
- You are dehydrated — signs of dehydration are excessive thirst, dry mouth, deep yellow urine or little or no urine, and severe weakness, dizziness, or light-headedness
- You notice blood in your bowel movements
- You have severe stomach pain
- You have a fever higher than 104 F (40 C)
For infants and children
Consult your child’s health care provider right away if your child:
- Has a fever of 102 F (38.9 C) or greater
- Seems tired or very irritable
- Has a lot of discomfort or pain
- Has bloody diarrhea
- Seems dehydrated — lookout for signs of dehydration in sick infants and children by comparing how much they drink and urinate with how much is normal for them, and watching for signs like a dry mouth, thirst, and crying without tears.
If you have an infant, remember that while spitting up might be an everyday occurrence for your baby, vomiting is not. Babies vomit for a variety of reasons, many of which might need medical attention.
Contact your baby’s doctor at once if your baby:
- Has vomiting that is frequent
- Has not had a wet nappy in 6 hours
- Has bloody stools or severe diarrhea
- Has a sunken soft spot (fontanel) on the top of the head
- Has a dry mouth or cries without the tears
- Is unusually sleepy, drowsy, or unresponsive
CAUSES
You are most likely to get viral gastroenteritis when you eat or drink contaminated food or water. You might also be likely to get gastroenteritis if you share utensils, towels, or food with someone who has one of the viruses that cause the condition.
Many viruses could cause gastroenteritis, including:
- Noroviruses – Both children and adults are affected by noroviruses, the most common cause of foodborne disease worldwide. Norovirus infection could sweep through families and communities. It is particularly likely to spread among people in confined spaces.
In the majority of cases, you pick up the virus from contaminated food or water. But it could also spread between people who are in close contact or who share food. You could also get the virus by touching a surface that has been contaminated with norovirus and then touching your mouth. - Rotavirus – Worldwide, this is the most common cause of viral gastroenteritis in children, who are generally infected when they put their fingers or other objects contaminated with the virus into their mouths. It could also spread through contaminated food. The infection is most serious in infants and young children.
Adults infected with rotavirus might not have symptoms but can still spread the disease. This is of particular concern in institutional settings like nursing homes because adults with the virus unknowingly could pass the virus to others. A vaccine against viral gastroenteritis is available in a few countries, including the United States, and seems to be effective in preventing the infection.
Some shellfish, particularly raw or undercooked oysters, also could make you sick. Contaminated drinking water is responsible for viral diarrhea. But in many cases, the virus is passed when someone with a virus handles the food you eat without washing his or her hands after using the washroom.
RISK FACTORS
Gastroenteritis happens all over the world and could affect people of all ages.
People who might be more susceptible to gastroenteritis include:
- Young children – Children in child care centers or elementary schools might be especially vulnerable because it takes time for a child’s immune system to mature.
- Older adults – Adult immune systems tend to become less effective later in life. Older adults in nursing homes are susceptible because their immune systems weaken. They also live in close contact with others who might pass along germs.
- Schoolchildren or dormitory residents – Anywhere that groups of people come together in close quarters could be an environment for an intestinal infection to get passed.
- Anyone with a weakened immune system – If your resistance to infection is low — for example, if your immune system is compromised by HIV/AIDS, chemotherapy, or another medical condition — you might be especially at risk.
Each gastrointestinal virus has a season in which it is most active. If you live in the Northern Hemisphere, for example, you are more likely to have rotavirus or norovirus infections in the winter and spring.

COMPLICATIONS
The primary complication of viral gastroenteritis is dehydration — a severe loss of water and essential salts and minerals. If you are healthy and drink enough to replace fluids you lose from vomiting and diarrhea, dehydration should not be a problem.
Infants, older adults, and people with weakened immune systems might become severely dehydrated when they lose more fluids than they could replace. Hospitalization may be needed so that lost fluids could be replaced through an IV in their arms. Dehydration could rarely lead to death.
PREVENTION
The most effective way to prevent the spread of intestinal infections is to follow these precautions:
- Get your child vaccinated – A vaccine against gastroenteritis caused by the rotavirus is available in a few countries, including the United States. Given to children in the first year of life, the vaccine seems to be effective in preventing severe symptoms of this disease.
- Wash your hands thoroughly – And ensure your children do, too. If your children are older, teach them to wash their hands, particularly after using the toilet.
Wash your hands after changing nappies and before preparing or eating food, too. It is best to use warm water and soap and to rub hands well for at least twenty seconds. Wash around cuticles, underneath fingernails, and in the creases of the hands. Then wash thoroughly. Carry sanitizing wipes and hand sanitizer for times when soap and water are not available. - Use separate personal items around your home – Do not share eating utensils, drinking glasses, and plates. Use separate bath towels in the bathroom.
- Prepare food safely – Wash all your fruits and vegetables prior to eating them. Clean kitchen surfaces prior to preparing food on them. Refrain from preparing food if you are ill.
- Keep your distance – Avoid close contact with anyone who has the virus, whenever possible.
- Disinfect hard surfaces – If someone in your home has viral gastroenteritis, disinfect hard surfaces, like counters, faucets, and doorknobs, with a mixture of 5-25 tablespoons (73 to 369 milliliters) of household bleach up to one gallon (3.8 liters) of water.
- Avoid touching laundry that may have been exposed to a virus – If a person from your home has viral gastroenteritis, wear gloves while touching the laundry. Wash clothing and bedding in hot water and dry them in the hottest setting. Wash your hands well after touching the laundry.
- Check out your child care center – Ensure the center has separate rooms for changing diapers and preparing or serving food. The area with the diaper-changing table should have a sink and a sanitary way to dispose of diapers.
Take precautions when traveling
When you are traveling in other countries, you could become ill from contaminated food or water. You might be able to reduce your risk by following these tips:
- Drink only well-sealed bottled or carbonated water.
- Avoid ice cubes because they might be made from contaminated water.
- Use bottled water to brush your teeth.
- Stay away from raw food — including peeled fruits, raw vegetables, and salads — that has been touched by human hands.
- Avoid undercooked meat and fish.

DIAGNOSIS
Your doctor will likely diagnose viral gastroenteritis (stomach flu) based on symptoms, a physical examination, and sometimes on the presence of similar cases in your community. A rapid stool test could detect rotavirus or norovirus, but there are no quick tests for other viruses that cause gastroenteritis. In some cases, your doctor might have you submit a stool sample to rule out a possible bacterial or parasitic infection.
TREATMENT
There is often no particular medical treatment for viral gastroenteritis. Antibiotics are not effective against viruses. Treatment first involves self-care measures, like staying hydrated.
If you or anyone you know is suffering from viral gastroenteritis, our expert providers at Specialty Care Clinics will take care of your health and help you recover.
Call us on (469) 545-9983 to book an appointment with our specialists.
