PULMONARY EDEMA: A LIFE-THREATENING CONDITION
With COVID-19 effects along with rising pollution, people often complain about the difficulty in breathing. However not all cases are serious and require clinical consideration, yet assuming you continually find it hard to breathe, gasp for breath generally with the issue turning out to be more awful when you rest, you should look for clinical assistance right away. It very well may be an indication of pulmonary edema!
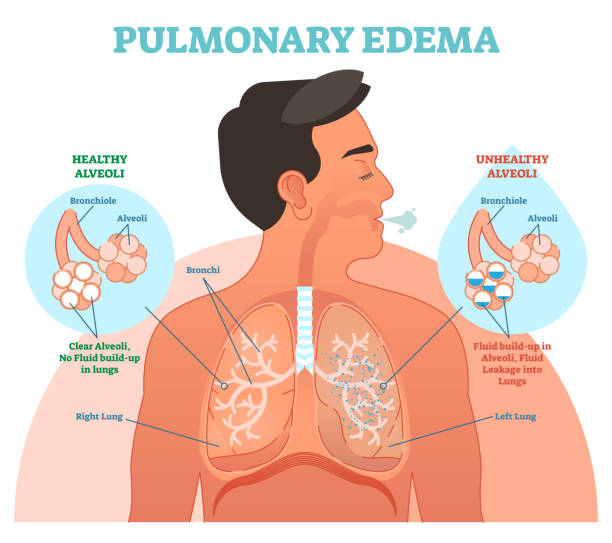
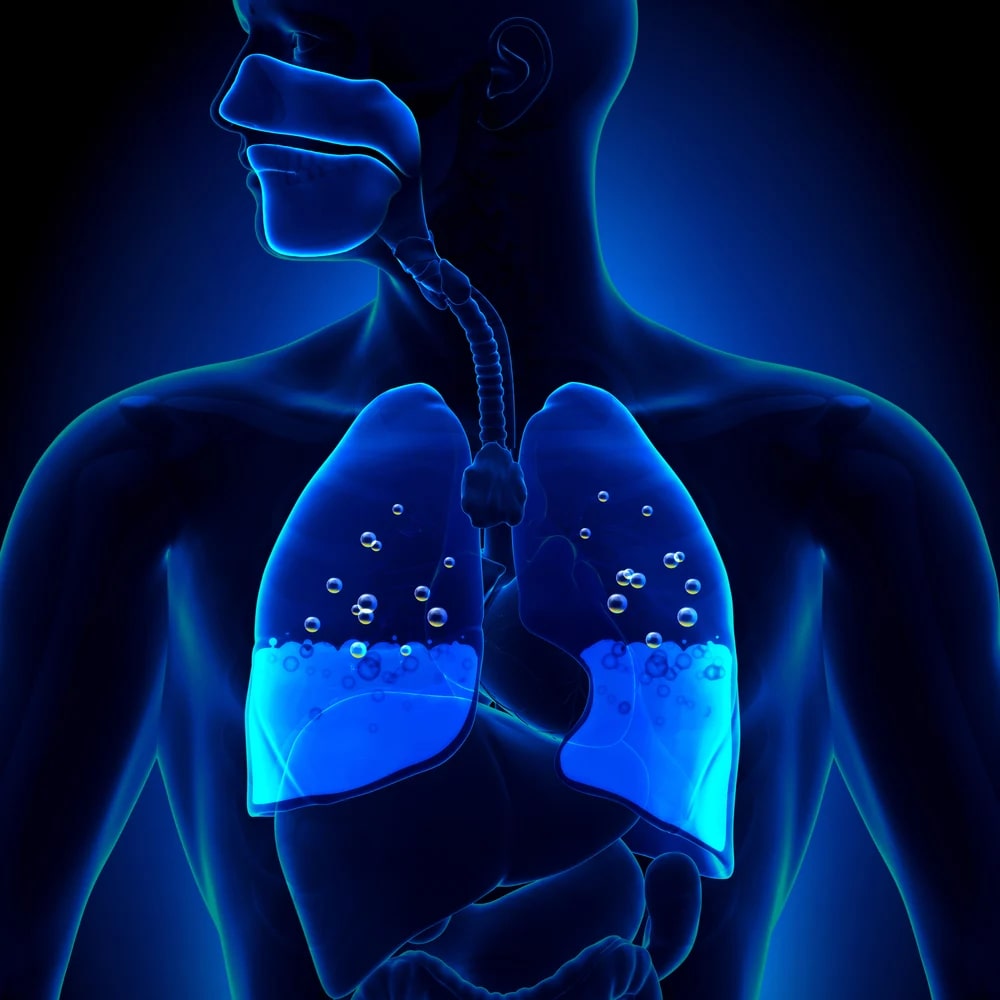
Pulmonary edema is a serious ailment that happens when excess fluid starts to fill the lungs’ air sacs (the alveoli). At the point when the alveoli are loaded up with fluid, they can’t satisfactorily add oxygen to or eliminate carbon dioxide from, the blood. So pulmonary edema produces huge breathing troubles, and may frequently turn into a life-threatening issue.
WHAT MAKES PULMONARY EDEMA A PROBLEM?
The alveoli are where the genuine work of the lungs happens. In the alveolar air sacs, the outside air we breathe comes in nearness to the vessels conveying oxygen-unfortunate blood from the body’s tissues. (This oxygen-unfortunate blood has quite recently been pumped from the right half of the heart out to the lungs, utilizing the pulmonary artery.)
Through the thin walls of the alveoli, an exchange of critical gas happens between the air within the alveolar sac and the “spent” blood within the vessels. Oxygen from the alveoli is taken up by the slender blood, and carbon dioxide from the blood diffuses into the alveoli. The blood, presently oxygen-rich by and by, is conveyed to the left half of the heart, which siphons it out to the tissues. The “utilized” alveolar air is breathed out to the environment, as we breathe. Life itself is reliant upon the productive trade of gasses within the alveoli.
With pulmonary edema, a portion of the alveolar sacs becomes loaded up with fluid. The critical trade of gasses between breathed in the air and slim blood can never again happen in the fluid-filled alveoli. Assuming adequate quantities of alveoli are impacted, serious side effects happen. Furthermore, assuming the pulmonary edema becomes extensive, death can follow.
WHAT LEADS TO PULMONARY EDEMA?
Doctors usually divide pulmonary edema into one of two types: cardiac pulmonary edema, and non-cardiac pulmonary edema.
- Cardiac Pulmonary Edema: Pulmonary edema is generally regularly caused because of congestive heart failure – when the heart can never again pump blood appropriately all through the body. This makes pressure on the small blood vessels of the lungs, which makes the vessels release fluid. At the point when fluid fills your lungs, they can’t place oxygen into the circulatory system, denying the remainder of the body the oxygen it needs. Cardiovascular pulmonary edema happens when a basic heart issue prompts pressures on the passed on side of the heart to become raised. This high strain is sent in reverse, through the pulmonary veins, to the alveolar vessels. On account of the raised pulmonary slim tension, fluid holes out of the vessels into the alveolar air space, and pulmonary edema happens.
- Non-cardiac Pulmonary Edema: For certain medical conditions, the alveoli can top off with fluid because of reasons inconsequential to raised heart pressure. This can happen when the vessels in the lungs become harmed, and as an outcome, they become “leaky” and permit fluid to enter the alveoli.
Some of the other medical reasons that might cause pulmonary edema include:
- Hypertension
- Heart diseases
- Damaged heart valves
- Pneumonia
- Sudden high blood pressure
- Kidney damage/failure
- Lung damage
Other external factors can cause pulmonary edema. These may include:
- High altitude exposure
- Drug overdose
- Lung damage caused by inhalation of toxins
- Severe trauma
- Major injury
HOW DO YOU IDENTIFY PULMONARY EDEMA?
Pulmonary edema symptoms might show up out of nowhere or substitute over the long haul. Symptoms rely upon the kind of pulmonary edema.
Sudden (acute) pulmonary edema symptoms:
- Difficulty breathing (dyspnea).
- Extreme shortness of breath worsens with activity or when lying down.
- The feeling of suffocating or drowning worsens when lying down.
- A cough that produces frothy sputum – may contain blood.
- A rapid, irregular heartbeat (palpitations).
- Anxiety, restlessness, or a feeling of something bad about to happen.
- Cold, clammy skin.
- Wheezing or gasping for breath.
Long-term (chronic) pulmonary edemam signs and symptoms
- Awakening at night with a cough or breathless feeling that may be relieved by sitting up
- Difficulty breathing while lying or doing the activity.
- Shortness of breath more than usual, mainly when you’re physically active.
- Fatigue.
- New or worsening cough.
- Fast weight gain.
- Swelling in the legs and feet.
- Wheezing.
High-altitude pulmonary edema (HAPE) signs and symptoms:
HAPE can happen in grown-ups and kids who travel to or practice at high heights. Symptoms of high-height pulmonary edema (HAPE) will generally deteriorate around evening time. Symptoms are like those that happen with intense pulmonary edema and can incorporate:
- Headache
- Shortness of breath with activity, which becomes shortness of breath at rest
- Not being able to exercise as much as you once could
- Dry cough, at first
- Later, a cough that produces frothy sputum that may look pink or have blood in it
- A very fast heartbeat (tachycardia)
- Weakness
- Chest pain
- Low fever
HOW DO DOCTORS DIAGNOSE PULMONARY EDEMA?
In the event that you experience the ill effects of any of the symptoms expressed over, it’s the ideal opportunity for you to get analyzed for pulmonary edema. Your doctors will search for fluid in your lungs, or symptoms brought about by its presence. For the finding, the patient would need to go through an actual assessment first. In the actual test, the specialist will utilize a stethoscope to look at the lungs for pops and quick breathing, and the heart for strange rhythms.
Your doctor might also:
- Check your neck for fluid buildup.
- Check your legs and abdomen for swelling.
- Check your skin for being pale or blue-colored.
- Discuss your symptoms and medical history in detail.
- Run some additional tests to check the fluid in your lungs.
Some of the tests your doctors can ask you to get done:
- Complete blood count
- Echocardiogram or an ultrasound – to check your heart activity.
- Chest X-ray – to see fluid.
- Blood tests – to check oxygen levels.
- ECG to look for heart problems or some other signs of a heart attack.
HOW TO TREAT PULMONARY EDEMA?
Pulmonary edema is a difficult condition that needs speedy treatment. Oxygen is the principal line of treatment on the off chance that you are experiencing pulmonary edema. Your medical care group would deliver 100% oxygen to you through an oxygen veil, nasal cannula, or positive tension cover.
Your PCP will likewise analyze the reason for pulmonary edema and afterward endorse the suitable treatment for the hidden reason.
On the basis of your condition, your doctor may also give:
- Preload reducers – to decrease pressures from the fluid going into your heart and lungs
- Afterload reducers – to dilate your blood vessels and take pressure off your heart
- Heart medications – to control your pulse, reduce hypertension, and relieve pressure in arteries and veins
- Morphine – to relieve anxiety and shortness of breath
When your condition is severe, your doctor may require intensive or critical care.
OUTLOOK
Pulmonary edema is a serious medical condition caused by excess fluid in the alveoli of the lungs. It is most often due to cardiac disease, but can also be produced by a range of non-cardiac medical problems. It is treated by rapidly addressing the underlying cause, using diuretics, and sometimes with mechanical ventilation.
People Also Read:
- Rare Lung Condition: Pneumothorax or Collapsed Lung
- Heart Attack Signs and Symptoms in Women
If you or anyone you know is suffering from septic arthritis, our expert providers at Specialty Care Clinics will take care of your health and help you recover.
Call us on 469-545-9983 to book an appointment with our specialists.