WHAT IS SEPTIC ARTHRITIS?
Septic arthritis is a painful infection in a joint that could come from germs that travel through your bloodstream from another part of your body. Septic arthritis could also occur when a penetrating injury, like an animal bite or trauma, delivers germs directly into the joint.
Infants and senior citizens are most likely to develop septic arthritis. People with artificial joints are also at risk for septic arthritis as well. Knees are most commonly affected, but septic arthritis also could affect hips, shoulders, and other joints. The infection could quickly and severely damage the cartilage and bone within the joint, so prompt treatment is crucial.
Treatment involves draining the joint with a syringe or during surgery. Antibiotics also are generally needed.
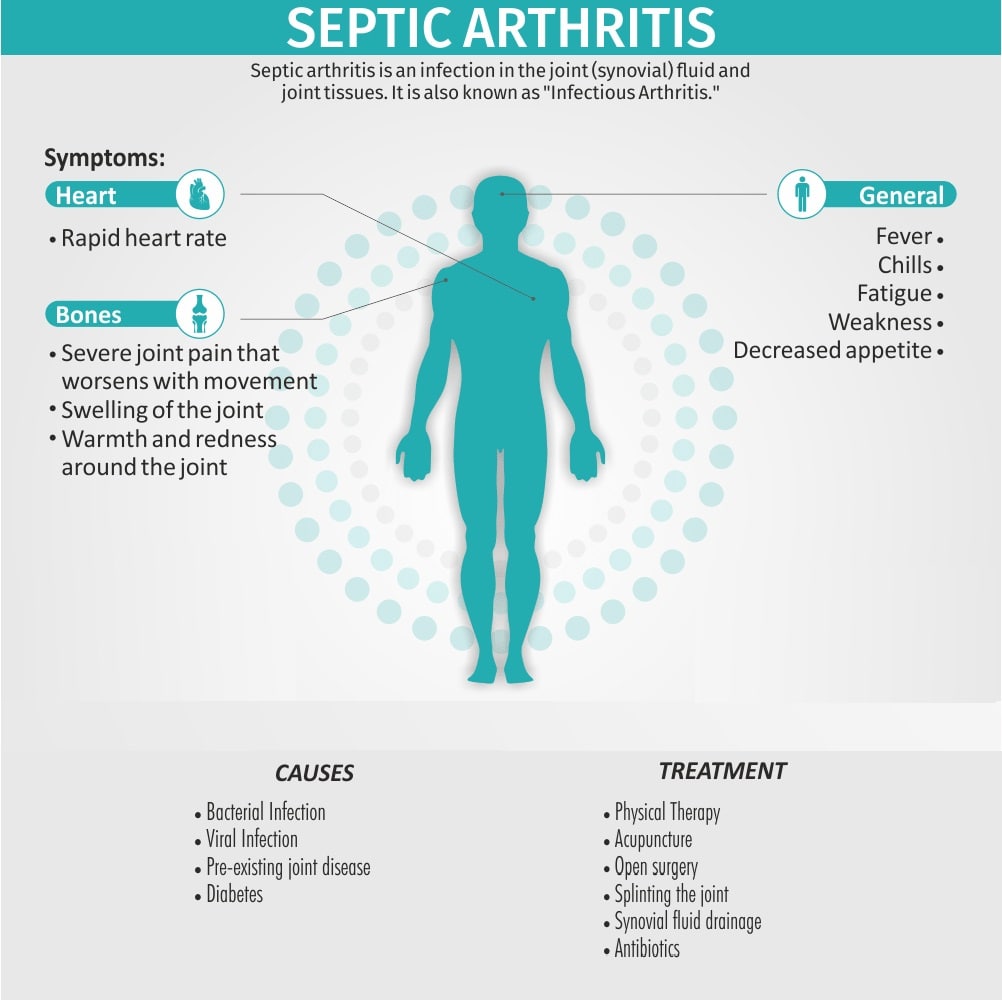
SYMPTOMS
Septic arthritis generally causes extreme discomfort and difficulty using the affected joint. The joint can be swollen, red and warm, and you might have a fever.
If septic arthritis occurs in an artificial joint (prosthetic joint infection), signs and symptoms like minor pain and swelling may develop months or years after knee replacement or hip replacement surgery. Also, a loosening of the joint might occur, which causes pain while moving the joint or while putting weight on the joint. Generally, the pain goes away when at rest. In extreme cases, the joint might become dislocated.
WHEN SHOULD YOU SEE A DOCTOR?
See your doctor if you have severe pain in a joint that comes on unexpectedly. Prompt treatment could help minimize joint damage.
If you have an artificial joint, consult your doctor if you experience pain while using the joint.
CAUSES
Septic arthritis could be caused by bacterial, viral, or fungal infections. Bacterial infection with Staphylococcus aureus (staph) is the most frequent cause. Staph frequently lives on even healthy skin.
Septic arthritis could develop when an infection, like a skin infection or urinary tract infection, spreads through your bloodstream to a joint. Less commonly, a puncture wound, drug injection, or surgery in or near a joint — including joint replacement surgery — could give the germs entry into the joint space.
The lining of your joints has little ability to protect itself against infection. Your body’s reaction to the infection — including inflammation that could increase pressure and reduce blood flow within the joint — contributes to the damage.
RISK FACTORS
Risk factors for septic arthritis include:
- Existing joint problem – Chronic diseases and conditions that affect your joints — like osteoarthritis, gout, rheumatoid arthritis, or lupus — could increase your risk of septic arthritis, as can previous joint surgery and joint injury.
- Having an artificial joint – Bacteria could be introduced during joint replacement surgery, or an artificial joint might become infected if germs travel to the joint from a different area of the body through the bloodstream.
- Taking medications for rheumatoid arthritis – People with rheumatoid arthritis have a further increase in risk because of medications they take that could suppress the immune system, making infections more likely to occur. Diagnosing septic arthritis in people with rheumatoid arthritis is difficult because many of the signs and symptoms are the same.
- Skin fragility – Skin that breaks easily and heals poorly could give bacteria access to your body. Skin conditions like psoriasis and eczema increase your risk of septic arthritis, as do infected skin wounds. People who regularly inject drugs also have a greater risk of infection at the site of injection.
- Weak immune system – People with weak immune systems are at higher risk of septic arthritis. This includes people with diabetes, kidney and liver issues, and those taking drugs that suppress their immune systems.
- Joint trauma – Animal bites, puncture wounds, or cuts over a joint could put you at risk of septic arthritis.
Having a combination of risk factors puts you at higher risk than having just one risk factor.
COMPLICATIONS
If treatment is delayed, septic arthritis could lead to joint degeneration and permanent damage. If septic arthritis affects an artificial joint, complications might include joint loosening or dislocation.
DIAGNOSIS
The following tests generally help diagnose septic arthritis:
- Joint fluid analysis – Infections could alter the color, consistency, volume, and makeup of the fluid within your joints. A sample of this fluid could be withdrawn from your affected joint with a needle. Laboratory tests could determine what organism is causing your infection, so your doctor will know which medications to prescribe.
- Blood tests – These could determine if there are signs of infection in your blood. A sample of your blood is removed from a vein with a syringe.
- Imaging tests – X-rays and other imaging tests of the affected joint could assess damage to the joint or loosening of an artificial joint.
A specialized scan that involves swallowing or injecting a small amount of a radioactive chemical might be used if your doctor suspects you have a prosthetic joint infection and it is been more than a year since you have had surgery.
TREATMENT
Doctors depend on joint drainage and antibiotic drugs to treat septic arthritis.
Joint drainage
Removing the infected joint fluid is important. Drainage methods include:
- Needle – In some cases, your doctor could withdraw the infected fluid with a needle inserted into the joint space.
- Scope procedure – In arthroscopy, a flexible tube with a video camera at its tip is placed in your joint through a tiny incision. Suction and drainage tubes are then inserted through tiny incisions around your joint.
- Open surgery – Some joints, like the hip, are more difficult to drain with a needle or arthroscopy, so an open surgical procedure might be necessary.
Antibiotics
To select the most effective medication, your doctor should identify the microbe causing your infection. Antibiotics are generally given through a vein in your arm at first. Later, you might be able to switch to oral antibiotics.
Generally, treatment lasts from two to six weeks. Antibiotics carry a risk of side effects such as nausea, vomiting, and diarrhea. Allergic reactions also could occur. Ask your doctor about what side effects to expect from your medicine.
Removal of replacement joint
If an artificial joint is infected, treatment usually involves removing the joint and temporarily replacing it with a joint spacer — a device made with antibiotic cement. After several months, a new replacement joint is implanted.
If a replacement joint cannot be removed, a doctor may clean the joint and remove damaged tissue but keep the artificial joint in place. Intravenous antibiotics are followed by oral antibiotics for several months in order to prevent the infection from coming back.
If you or anyone you know is suffering from septic arthritis, our expert providers at Specialty Care Clinics will take care of your health and help you recover.
Call us on 469-545-9983 to book an appointment with our specialists.