WHAT IS WHIPPLE’S DISEASE?
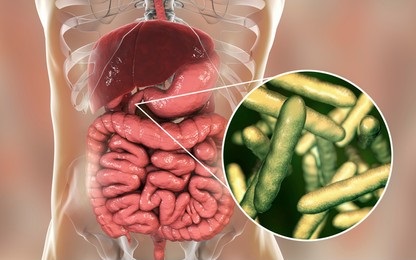
Whipple disease is an unusual bacterial infection that most usually affects your joints and digestive system. Whipple disease intervenes with normal digestion by impairing the breakdown of foods and hampering your body’s ability to absorb nutrients, like fats and carbohydrates.
Whipple disease could also infect other organs, including your brain, heart, and eyes.
Without proper treatment, Whipple’s disease could be severe or fatal. Although, a course of antibiotics could treat Whipple disease.
WHIPPLE’S DISEASE SYMPTOMS
Common signs and symptoms
Digestive signs and symptoms are common in Whipple disease and might include:
- Diarrhea
- Abdominal cramping and pain, which might worsen after meals
- Weight loss, related to the malabsorption of nutrients
Other common signs and symptoms related to Whipple disease include:
- Inflamed joints, especially the ankles, knees, and wrists
- Fatigue
- Weakness
- Anemia
Less common signs and symptoms
In some cases, signs and symptoms of Whipple disease might include:
- Fever
- Cough
- Enlarged lymph nodes
- Skin darkening in regions exposed to the sun and in scars
- Chest pain
Brain and nervous system (neurological) signs and symptoms might include:
- Trouble walking
- Vision issues, including lack of control of eye movements
- Confusion
- Memory loss
Symptoms tend to develop gradually over many years in most people with this disease. In some people, symptoms like joint pain and weight loss develop years before the digestive symptoms that lead to the diagnosis.
WHEN SHOULD YOU SEE A DOCTOR?
Whipple disease is potentially life-threatening yet generally treatable. Contact your doctor or primary care physician if you experience uncommon signs or symptoms, like unexplained weight loss or joint pain. Your doctor or primary care physician could perform tests to determine the cause of your symptoms.
Even after the infection is diagnosed and you are receiving treatment, let your doctor or primary care physician know if your symptoms do not improve. Sometimes antibiotic therapy is not effective because the bacteria are resistant to the particular drug you are taking. The disease could recur, so it is important to watch for symptoms that reappear.
WHIPPLE’S DISEASE CAUSES
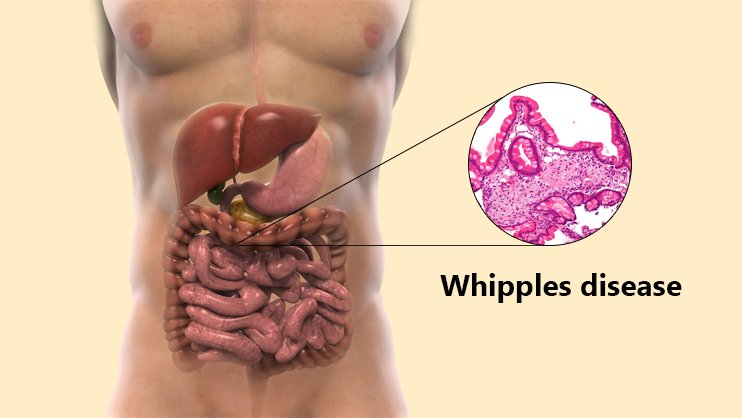
Whipple disease is caused by a type of bacterium known as Tropheryma whipplei. The bacteria damage the mucosal lining of your small intestine first, forming small sores (lesions) inside the wall of the intestine. Bacteria also affect the fine, hair-like projections (villi) that line the small intestine.
There is not a lot we know about bacteria. However, they seem readily present in the environment, scientists do not know where they come from or how they are spread to humans. Not everyone who carries the bacteria develops this illness. Some researchers believe that people with the disease might have a genetic defect in their immune system response that makes them more likely to become ill when exposed to the bacteria.
Whipple’s disease is very rare, affecting fewer than 1 in 1 million people.
WHIPPLE’S DISEASE RISK FACTORS
Because so little is known about the bacteria that cause Whipple disease, risk factors for the disease have not been clearly identified. Based upon available reports, it appears more likely to affect:
- Men ages 40 years to 60 years
- White people in North America and Europe
- Farmers and other people who work outdoors and have common contact with sewage and wastewater
WHIPPLE’S DISEASE COMPLICATIONS
The lining of your small intestine has fine, hair-like projections (villi) that help your body to absorb nutrients. Whipple disease affects the villi, impairing nutrient absorption. Nutritional deficiencies are frequent in people with Whipple disease and could lead to fatigue, weakness, weight loss, and joint pain.
Whipple disease is a progressive and possibly fatal disease. However, the infection is unusual, related deaths continue to be reported. This is due in large part to late diagnosis and delayed treatment. Death usually is caused by the spread of the infection to the central nervous system, which could cause irreversible damage.
WHIPPLE’S DISEASE DIAGNOSIS
The process of diagnosing Whipple disease generally includes the following tests:
Physical examination – Your doctor or primary care physician generally starts with a physical examination. He or she will look for signs and symptoms that indicate the presence of this condition. For instance, your doctor or primary care physician might look for stomach tenderness and skin darkening, especially on sun-exposed parts of your body.
Biopsy – An important step in diagnosing Whipple disease is taking a tissue sample (biopsy), generally from the lining of the small intestine. To do this, your doctor or primary care physician usually performs an upper endoscopy. The endoscopy procedure uses a thin, flexible tube (scope) with a light and a small camera attached that passes through your mouth, throat, windpipe, and stomach to your small intestine. The scope enables your doctor or primary care physician to view your digestive passages and take tissue samples.
- During the procedure, doctors or primary care physicians remove tissue samples from several areas in the small intestine. A doctor or primary care physician examines this tissue under a microscope in a laboratory. He or she looks for the presence of disease-causing bacteria and their sores (lesions), and particularly for Tropheryma whipplei bacteria. If these tissue samples do not confirm the diagnosis, your doctor or primary care physician may take a tissue sample from an enlarged lymph node or perform other tests.
- In some cases, your doctor or primary care physician might ask you to swallow a capsule that holds a small camera. The camera could take pictures of your digestive passages for your doctor or primary care physician to view.
- A DNA-based test called a polymerase chain reaction, which is available at some medical centers, could detect Tropheryma whipplei bacteria in biopsy specimens or spinal fluid samples.
Blood tests – Your doctor or primary care physician might also order blood tests, like a complete blood count. Blood tests could detect specific conditions related to Whipple disease, specifically anemia, which is a decline in the number of red blood cells, and low concentrations of albumin, a protein in your blood.
WHIPPLE’S DISEASE TREATMENT
Treatment of Whipple disease is with antibiotics, either alone or in combination, which could destroy the bacteria causing the infection.
Treatment is long-term, usually lasting a year or two, with the aim of destroying the bacteria. But symptom relief usually comes much quicker, generally within the first week or two. Most people with no brain or nervous system complications recover fully after a full course of antibiotics.
When choosing antibiotics, doctors or primary care physicians usually select those that wipe out infections in the small intestine and also cross a layer of tissue around your brain (the blood-brain barrier). This is done to eliminate bacteria that might have entered your brain and central nervous system.
Because of the lengthy use of antibiotics, your doctor or primary care physician will need to monitor your condition for the development of resistance to the drugs. If you relapse during treatment, your doctor or primary care physician might change your antibiotics.
Treatment for standard cases
In most cases, Whipple disease therapy starts with two to four weeks of ceftriaxone or penicillin given through a vein in your arm. Following that initial therapy, you will likely take an oral course of sulfamethoxazole-trimethoprim (Bactrim, Septra) for one to two years.
Potential side effects of ceftriaxone and sulfamethoxazole-trimethoprim include allergic reactions, mild diarrhea, or nausea, and vomiting.
Other medications that have been recommended as an alternative in some cases include oral doxycycline (Vibramycin, Doryx, others) combined with the antimalarial drug hydroxychloroquine (Plaquenil), which you will likely need to take for one to two years.
Potential side effects of doxycycline include loss of appetite, nausea, vomiting, and sensitivity to sunlight. Hydroxychloroquine might cause loss of appetite, diarrhea, headache, stomach cramps, and dizziness.
Symptom relief
Your symptoms should improve within one to two weeks of starting antibiotic treatment and go away completely within about one month.
But even though symptoms improve quickly, further laboratory tests might reveal the presence of the bacteria for two or more years after you start taking antibiotics. Follow-up testing will help your doctor or primary care physician determine when you could stop taking antibiotics. Regular monitoring could also detect the development of resistance to a particular drug, usually indicated by a lack of improvement in symptoms.
Even after successful treatment, Whipple disease could recur. Doctors or primary care physicians generally advise regular check-ups. If you have experienced a recurrence, you will need to repeat antibiotic therapy.
Taking supplements
Because of the nutrient-absorption difficulties related to Whipple disease, your doctor or primary care physician might suggest taking vitamin and mineral supplements to ensure adequate nutrition. Your body might need additional vitamin D, folic acid, calcium, iron, and magnesium.
If you or anyone you know is suffering from Whipple’s disease, our expert providers at Specialty Care Clinics will take care of your health and help you recover.
Call (469) 545-9983 to book a telehealth appointment for an at-home check-up.
