What is Retrolisthesis?
The spinal condition retrolisthesis is the opposite of spondylolisthesis. While both disorders include a vertebral body slipping over the one below, the difference is directional. Retrolisthesis is a rearward or backward slippage, and spondylolisthesis (sometimes known as anterolisthesis) is a frontward or forward slip. Another terminology for either disorder is vertebral displacement. Of the two, retrolisthesis is uncommon.
Both disorders could develop at any vertebral level in the spinal column, however the cervical (neck) and lumbar (low back) areas are more common. The neck is exposed to stresses as it supports the head at rest and during different movements. Although, the lumbar spine maintains the body’s weight, and absorbs and distributes forces while at rest and during physical function.
A retrolisthesis might include the spine’s vertebra, discs, ligaments, tendons or fascia, muscles, and nerves. It might cause symptoms associated with other spinal conditions, like spinal stenosis, facet joint dysfunction, cauda equina syndrome (lumbar spine), and intervertebral disc bulge or herniation.
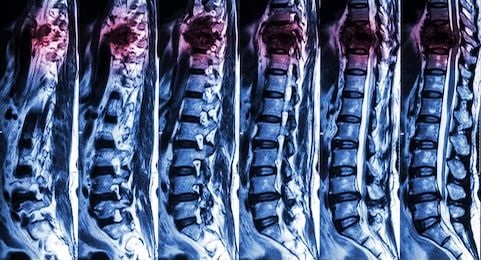
Types of Retrolisthesis
- Complete retrolisthesis – A vertebra slips backward or rearwards between the spinal segment above and beneath it.
- Partial retrolisthesis – A vertebra slips backward or rearwards to either the spinal segment above or beneath it.
- Stair-stepped retrolisthesis – A vertebra slips backward or rearwards to the spinal segment above it and ahead of the one beneath it.
Retrolisthesis Grades
Just like spondylolisthesis, the seriousness of a retrolisthesis is graded from 1 to 4 based upon the percentage of posterior or backward displacement of the vertebral body’s foramen or neuroforamen. The grade of a retrolisthesis is crucial to evaluating the stability of the adjacent facet joint.
- Grade 1: Up to 25%
- Grade 2: 25% to 50%
- Grade 3: 50% to 75%
- Grade 4: 75% to 100%
Retrolisthesis Symptoms
Retrolisthesis symptoms alter greatly and depend, in part, upon the grade of vertebral displacement and how the adjacent structures are damaged by the posterior or backward slippage.
- Pain in the area of the vertebral displacement intensity, frequency and description are changed (for example, dull, sharp)
- The displacement might be palpable or felt by hand
- Range of motion movement lowered
- Neurological symptoms like weakness, numbness, or tingling feelings at the area of displacement and/or spread into other parts of the body (for example, shoulders, arms, buttocks, hips, legs)
Retrolisthesis Causes
There are different spine associated problems which could cause or contribute to the development of retrolisthesis. The partial list below are conditions which could affect the spine’s structures that being, the individual anatomical parts (for example, bones, ligaments) which help maintain the spine’s stability and normal function.
- Degenerative spinal disorders (, degenerative disc disease)
- Arthritis (for example, spondylosis, osteoarthritis)
- Osteoporosis
- Spinal injury (for example, spinal cord injury, fracture)
- Muscle weakness in the abdomen and/or spine
- Infections of the blood
- Osteomyelitis or (bone infection)
- Birth defects
- Nutritional deficiencies
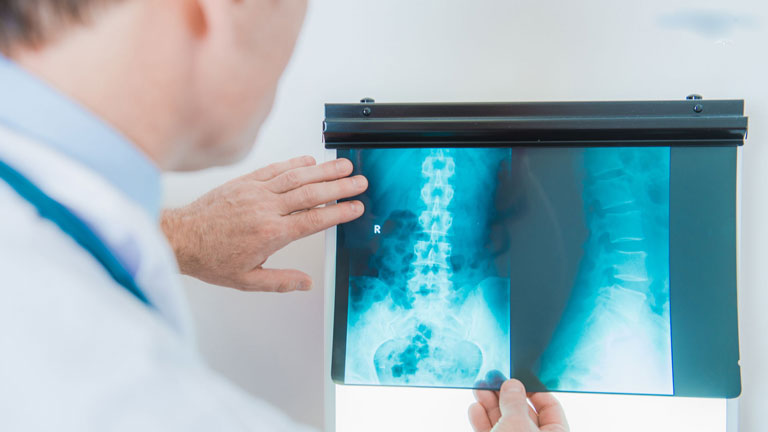
Retrolisthesis Diagnosis
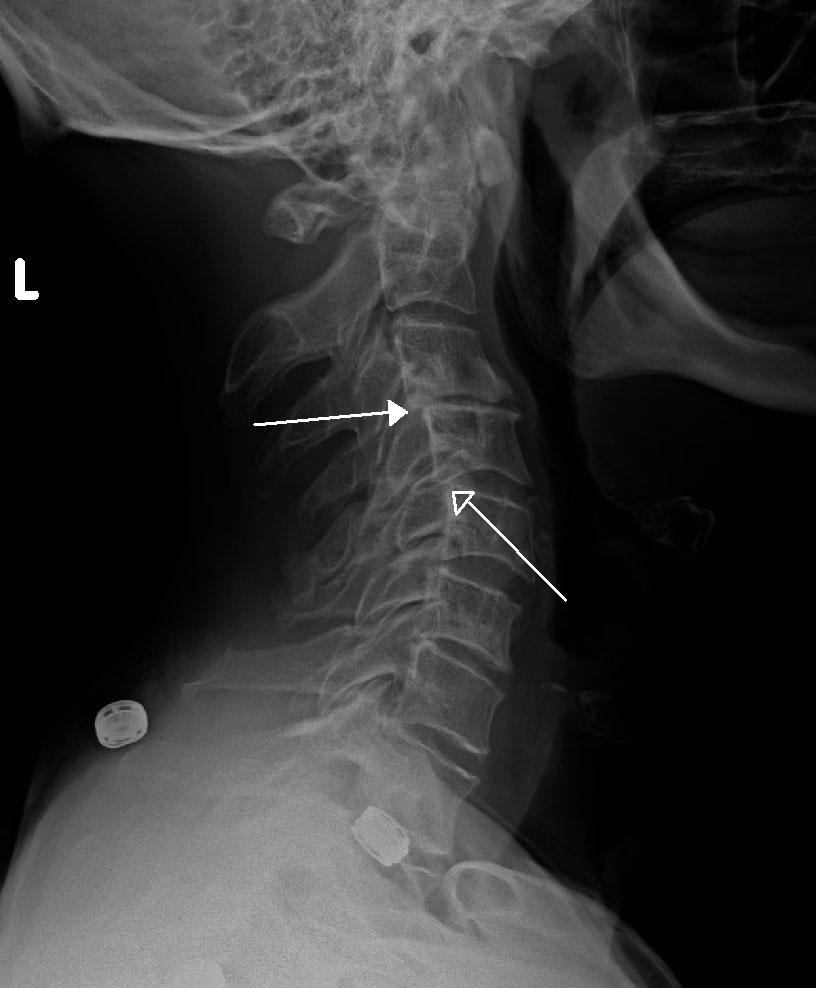
The diagnosis of retrolisthesis includes a physical exam and neurological assessment which involve details about your medical history and symptoms. Afterwards, standing x-ray imaging of your spine is performed (for example, anterior, posterior, lateral).The retrolisthesis might be viewed on the x-ray or other imaging study.
Using the image, your primary care physician could measure its displacement (how far out of normal position). If the displacement is more than 2 mm, your primary care physician might diagnose you with retrolisthesis (for example, Grade 1). Depending upon the results of your neurological examination and review of symptoms, your primary care physician might order additional imaging tests, like a CT or MRI scan.
Retrolisthesis Treatment
If your primary care physician informs you that one of your vertebrae has slipped posterior or backward, you might immediately assume that spine surgery is your only alternative. There are many considerations before advancing to surgery, like the retrolisthesis grade, stability of the slip and its risk for progression, symptom seriousness, and your response to non-operative therapies. Surgery is rarely required.
Non-surgical treatments might include a single therapy or a combination, and are usually successful at managing the swelling, pain and related symptoms:-
- Pain medication, like non-steroidal anti-inflammatory drugs (NSAIDs), to lower swelling, relieve pain
- Muscle relaxant medication
- Spinal injections
- Ice, heat
- Modification of physical activities which exacerbate pain and symptoms
- Massage
- Physical therapy; passive (for example, massage, ultrasound) and active (exercise) treatments
- Walking, swimming, yoga under primary care physician’s guidance
If spine surgery is suggested, your primary care physician will explain exactly why it is required, the surgical goals and type of techniques. For instance, a progressive or high grade retrolisthesis might need spinal stabilization using instrumentation and spinal fusion to stop the disorder from worsening. As mentioned earlier, retrolisthesis could cause other complications, like spinal stenosis which might need surgical decompression (for example, laminectomy) to ease nerve impingement.
Your primary care physician might recommend nutritional support to improve and sustain your bone and joint health. Certain vitamins, like vitamins A, C, and D, and nutrients like calcium and protein could be integral to long-term spine health.
The most important point in preserving your quality of life with retrolisthesis is to follow your primary care physician’s guidance. Staying active, eating a healthy diet rich in nutrients, and taking care to stop spinal injury go a long way toward helping to manage this disorder.
If you or anyone you know is suffering from retrolisthesis, our expert providers at Specialty Care Clinics will take care of your health and help you recover.
