WHAT IS PELVIC GIRDLE PAIN?
Pelvic girdle pain (PGP) is a group of symptoms that cause discomfort in the pelvic region. It generally happens during pregnancy, when your pelvic joints become stiff or move unevenly. It could happen both at the front and back of your pelvis. Pelvic girdle pain (PGP) is also sometimes referred to as symphysis pubis dysfunction (SPD).
The condition is not harmful to your baby, but it can be extremely painful for you. In some, the pain might be so serious that it affects mobility.
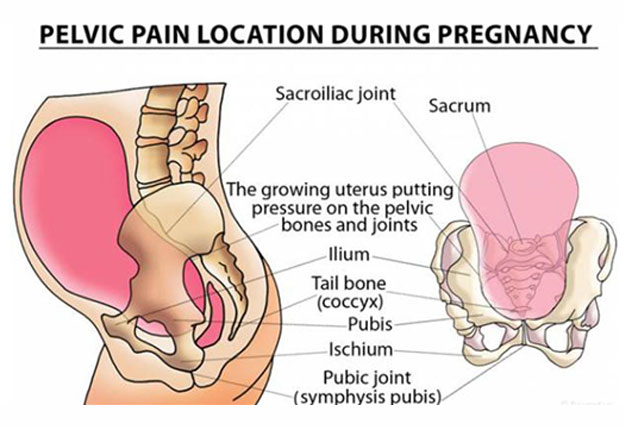
PELVIC GIRDLE PAIN SYMPTOMS
The symptoms of pelvic girdle pain (PGP) could differ for different people, both in terms of severity and presentation. The most commonly experienced symptoms include:
- Pain in the middle before the pubic bone
- Pain in the lower back on one or two sides.
- Pain in your perineum, the region between the anus and vagina
- The pain sometimes moves towards your thighs, and you might also hear or feel a grinding or popping sound in your pelvis.
The pain is usually more obvious when you are:
- Walking
- Using stairs
- Putting your weight on one leg
- Turning over in your bed
It may also be challenging to widen your legs. This could make everyday tasks like getting out of bed, getting dressed, or getting in and out of a car difficult.
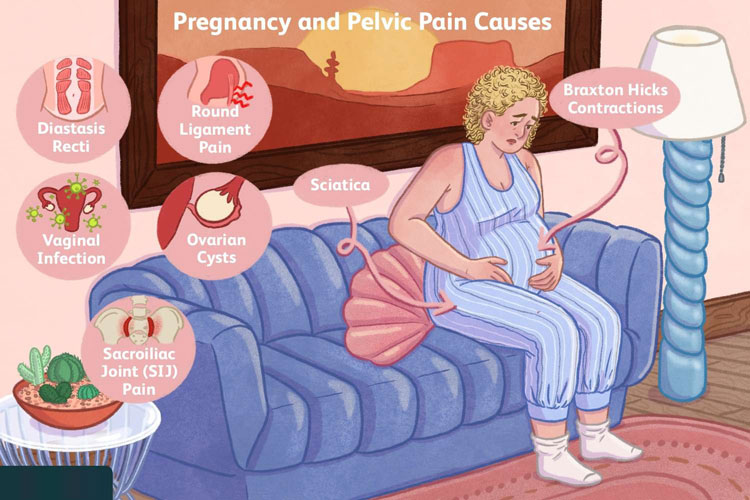
PELVIC GIRDLE PAIN CAUSES
The most common cause of pelvic girdle pain (PGP) is pregnancy. It is thought that pelvic girdle pain (PGP) affects up to one in five pregnant women to some extent.
During pregnancy, hormones like relaxin are released to loosen the ligaments and muscles in your:
- Hips
- Stomach
- Pelvic floor
- Pelvis
This slackening is intended to raise your extent of motion in order to help you give birth, but it also means that your joints could become unbalanced and more mobile than they generally would be. This could cause discomfort or pain.
However this slackening is intended to help with the birth, sometimes you could start producing these hormones in early pregnancy. You might experience the symptoms of pelvic girdle pain (PGP) long before it is time to give birth.
The baby’s weight and position are also believed to have an effect on pelvic pain. The symptoms of pelvic girdle pain (PGP) tend to worsen as the pregnancy progresses.
It is much less common for pelvic girdle pain (PGP) to happen outside of pregnancy, but it does happen. Other causes of pelvic girdle pain (PGP) range from pelvic injuries to conditions like osteoarthritis. In some instances, no known cause exists.

PELVIC GIRDLE PAIN PREVENTION
There is very little that you could do to prevent yourself from getting pelvic girdle pain (PGP) in pregnancy. Although, it is more common if you have had a previous pelvic injury, so it is always important to take whatever measures possible to protect this important region of your body.
PELVIC GIRDLE PAIN DIAGNOSIS
Early diagnosis could be really helpful in managing pelvic girdle pain (PGP). If you are pregnant and experiencing pelvic pain, talk to your doctor or primary care physician, or healthcare provider. They will be able to refer you to a physiotherapist who could assess the stability and strength of your joints and pelvic muscles. They will also help you plan what activities you will be able to do.
COULD IT LEAD TO PREGNANCY COMPLICATIONS?
Pelvic girdle pain (PGP) is not medically harmful to your baby, and most women with the state are still able to deliver vaginally. Although, chronic pain could lead to sadness or even depression, which is sometimes thought to have a negative effect on your baby.
However, the symptoms of pelvic girdle pain (PGP) do not tend to go away completely till you have given birth, there are lots of things that could be done to reduce your pain. That is why it is important to look for help.
The Pelvic, Obstetric, and Gynaecological Physiotherapy group from the United Kingdom (UK) suggest that you try to avoid the following activities if you are experiencing pelvic girdle pain (PGP):
- Putting your weight on only one leg
- Twisting and bending while lifting
- Carrying a child on your hip
- Crossing your legs
- Sitting on the floor
- Sitting in a twisted position
- Remain standing and sitting for extended periods of time.
- Lifting heavy loads, like wet laundry, shopping bags, or a toddler
- Vacuuming
- Pushing heavy objects, like a shopping cart
- Carrying anything in only one hand
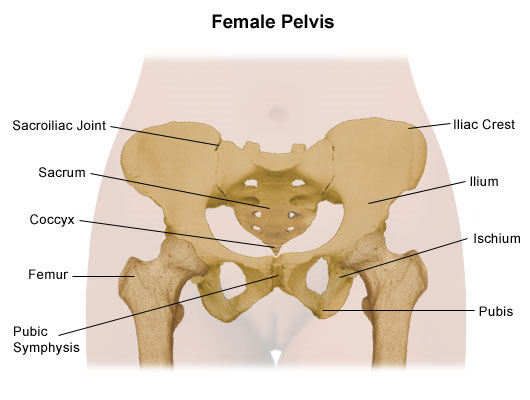
PELVIC GIRDLE PAIN TREATMENT
Physiotherapy is the first course of treatment for pelvic girdle pain (PGP). The goal of physiotherapy is to:
- Minimize your pain
- Improve your muscle function
- Improve your pelvic joint stability and position
A physiotherapist could provide manual therapy to make sure that the joints in your pelvis, spine, and hips move normally. They will also be able to offer you exercises to strengthen the muscles in your pelvic floor, back, stomach, and hips.
They might recommend hydrotherapy, where you do the exercises in the water. Being in the water could take the stress off your joints and permit you to move more easily. The physiotherapist will be able to give you recommendations on comfortable positions for sex, labor, and birth.
In serious cases of pelvic girdle pain (PGP), pain medications or transcutaneous electrical nerve stimulation (TENS) therapy might be prescribed. You might also be provided with supportive equipment like crutches or pelvic support belts. Application of heat or cold to the region might reduce pain or inflammation.
CONCLUSION
Pelvic girdle pain (PGP) does not directly affect your baby, but it might lead to a more difficult pregnancy because of reduced mobility. Some women might also have difficulty having a vaginal delivery.
Symptoms of pelvic girdle pain (PGP) usually reduce after giving birth. Talk to your doctor or primary care physician if your symptoms still do not improve. They could check if they might be the result of another hidden condition.
If you or anyone you know is suffering from pelvic girdle pain, our expert providers at Specialty Care Clinics will take care of your health and help you recover.
Call 469-545-9983 to book a telehealth appointment for an at-home check-up.
