WHAT IS NAIL FUNGUS?
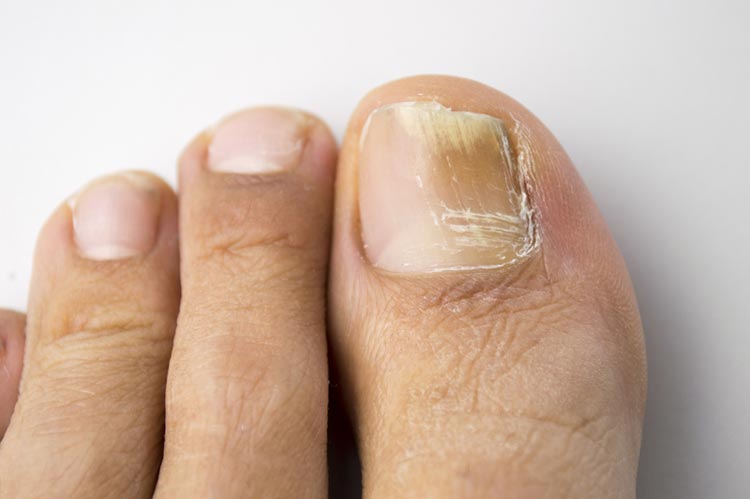
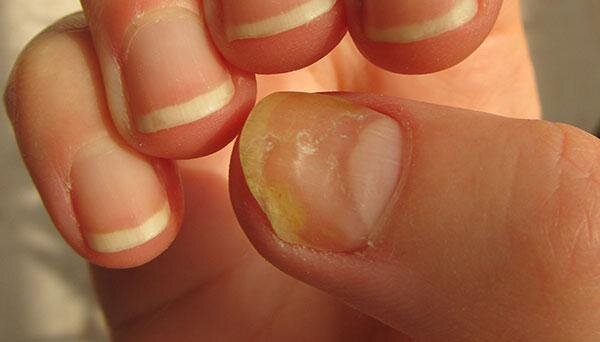
Nail fungus is a normal condition that starts as a white or yellow spot under the tip of your fingernail or toenail. As the fungal infection goes deeper, nail fungus might cause your nail to discolor, thicken and crumble at the edge. It could affect several nails.
If your condition is mild and not bothering you, you might not require treatment. If your nail fungus is painful and has caused thickened nails, self-care steps and medicines might help. But even if the treatment is successful, nail fungus frequently returns.
Nail fungus is also known as onychomycosis. When fungus infects the regions between your toes and the skin of your feet, it is known as the athlete’s foot (tinea pedis).
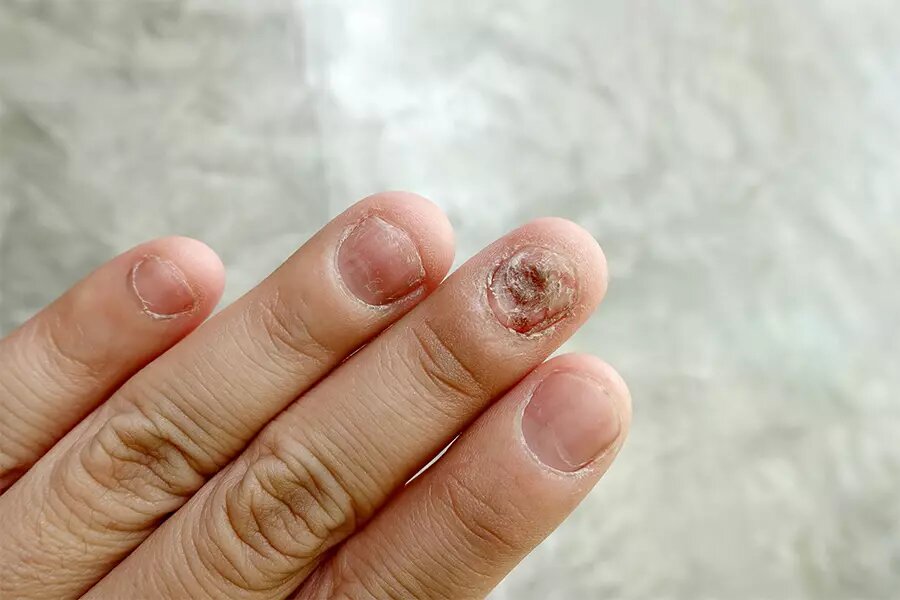
NAIL FUNGUS SYMPTOMS
You might possibly have nail fungus if one or more of your nails are:
- Thickened
- Whitish to yellow-brown discoloration
- Brittle, crumbly, or ragged
- Distorted in shape
- A dark color, because of debris building up under your nail
- Smelling slightly foul
- Nail fungus could affect fingernails, but it is more common in toenails.
- Healthy Lungs
WHEN SHOULD YOU SEE A DOCTOR?
You might want to see a physician if self-care steps have not helped and the nail becomes increasingly discolored, thickened, or deformed. Also, see a doctor or primary care physician if you have diabetes and think you are developing nail fungus.
NAIL FUNGUS CAUSES
Fungal nail infections are due to various fungal organisms (fungi). The most common cause is a form of fungus known as dermatophyte. Yeast and molds also could cause nail infections.
Fungal nail infection could develop in people at any age, but it is more common in older adults. As the nail ages, it could become brittle and dry. The resulting cracks in the nails permit fungi to come in. Other factors like lowered blood circulation to the feet and a weakened immune system also might play a role.
Toenail fungal infection could begin from the athlete’s foot (foot fungus), and it could spread from one nail to another. But it is rare to get an infection from someone else.
NAIL FUNGUS RISK FACTORS
Factors that could increase your risk of developing nail fungus include:
- Being older, owing to lowered blood flow, more years of exposure to fungi, and slower growing nails
- Sweating heavily
- Having a history of athlete’s foot
- Walking barefoot in damp communal regions, like swimming pools, gyms, and shower rooms
- Having a minor skin or nail injury or a skin condition, like psoriasis
- Having diabetes, circulation issues, or a weakened immune system
NAIL FUNGUS COMPLICATIONS
A serious case of nail fungus could be painful and might cause permanent damage to your nails. And it might lead to other severe infections that spread beyond your feet if you have a suppressed immune system because of medicine, diabetes, or other conditions.
If you have diabetes, you might have lowered blood circulation and nerve supply in your feet. You are also at higher risk of a bacterial skin infection (cellulitis). So any relatively minor injury to your feet including a nail fungal infection could lead to a more severe complication. See your doctor or primary care physician if you have diabetes and think you are developing nail fungus.
NAIL FUNGUS PREVENTION
The following habits could help prevent nail fungus or infections and athlete’s foot, which could lead to nail fungus:
- Wash your hands and feet daily. Clean your hands after touching an affected nail. Hydrate your nails after washing.
- Trim nails straight across, smooth the edges with a file, and file down thickened regions. Clean your nail clippers after each use.
- Wear sweat-absorbing socks or change your socks every day.
- Choose shoes made of materials that breathe.
- Dispose of old shoes or treat them with disinfectants or antifungal powders.
- Wear footwear in pool regions and locker rooms.
- Choose a nail salon that uses cleaned manicure tools for each customer.
- Give up nail polish and artificial nails.
NAIL FUNGUS DIAGNOSIS
Your doctor or primary care physician will examine your nails. He or she might also take some nail clippings or scrape debris from under your nail and send the sample to a laboratory to identify the type of fungus causing the infection.
Other conditions, for example, psoriasis, could mimic a fungal infection of the nail. Microorganisms like yeast and bacteria also could infect nails. Knowing the cause of your infection helps decide the best course of treatment.
NAIL FUNGUS TREATMENT
Fungal nail infections could be difficult to treat. Talk with your doctor or primary care physician if self-care strategies and over-the-counter (non-prescription) products have not helped. Treatment depends on the seriousness of your condition and the form of fungus causing it. It could take months to see results. And even if your nail condition gets better, repeat infections are common.
Medications
Your doctor or primary care physician might prescribe anti-fungal drugs that you take orally or apply to the nail. In some situations, it helps to combine oral and topical anti-fungal treatments.
- Oral antifungal drugs – These drugs are usually the first choice because they clear the infection more rapidly than do topical drugs. Alternatives include terbinafine (Lamisil) and itraconazole (Sporanox). These drugs help a new nail grow free of infection, gradually replacing the infected part.
- You generally take this type of drug for six to twelve weeks. But you would not see the end result of treatment until the nail grows back completely. It might take 4 months or longer to eliminate an infection. Treatment success rates with these drugs appear to be lower in adults over age 65 years.
- Oral antifungal drugs might cause side effects ranging from skin rash to liver damage. You might require occasional blood tests to check on how you are doing with these types of drugs. Doctors or primary care physicians might not recommend them for people with liver disease or congestive heart failure or those taking specific medications.
- Medicated nail polish – Your doctor or primary care physician might prescribe an anti-fungal nail polish known as ciclopirox (Penlac). You paint it on your affected nails and surrounding skin once a day. After 7 days, you wipe the piled-on layers clean with alcohol and start fresh applications. You might require to use this type of nail polish daily for almost a year.
- Medicated nail cream – Your doctor or primary care physician might prescribe an anti-fungal cream, which you rub into your affected nails after soaking. These creams might work better if you first thin the nails. This helps the medication get through the hard nail surface to the hidden fungus.
- To thin nails, you apply a non-prescription lotion containing urea. Or your doctor or primary care physician might thin the surface of the nail (debride) with a file or other tool.
Surgery
Your doctor or primary care physician may recommend temporary removal of the nail so that he or she could apply the anti-fungal drug directly to the infection under the nail.
Some fungal nail infections do not respond to medicines. Your doctor or primary care physician may recommend permanent nail removal if the infection is severe or extremely painful.
If you or anyone you know is suffering from nail fungus, our expert providers at Specialty Care Clinics will take care of your health and help you recover.
Call 469-545-9983 to book a telehealth appointment for an at-home check-up.
