WHAT IS KAWASAKI DISEASE?
Kawasaki disease causes swelling (protrusion) in the walls of middle-sized arteries across the body. It mainly affects children. The inflammation tends to damage the coronary arteries, which deliver blood to the heart muscle.
Kawasaki disease is otherwise known as mucocutaneous lymph node syndrome as it also damages glands that inflame during an infection (lymph nodes), skin, and the mucous membranes inside the mouth, nose, and throat.
Signs of Kawasaki disease, for example, high fever and peeling skin, could be frightening. The good news is that Kawasaki disease is generally treatable, and most children heal from Kawasaki disease without severe issues.
KAWASAKI DISEASE SYMPTOMS
Kawasaki disease signs and symptoms generally appear in three phases.
1st phase
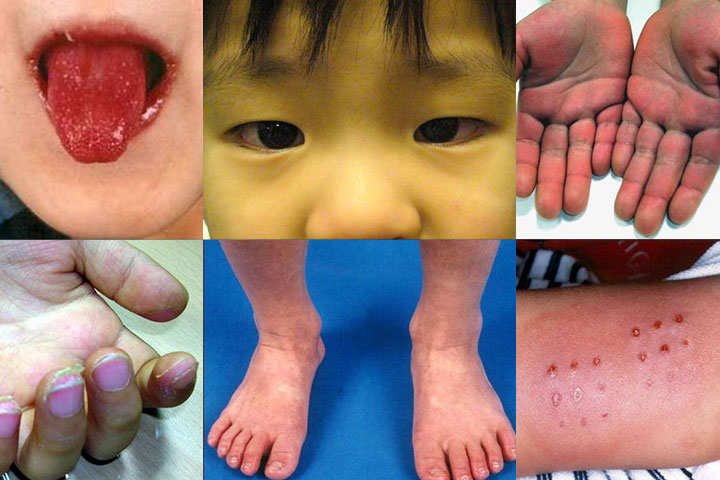
Signs and symptoms of the first phase might include:
- A fever that is usually is higher than 102.2 F (39 C) and lasts more than 3 days
- Extremely red eyes with no heavy discharge
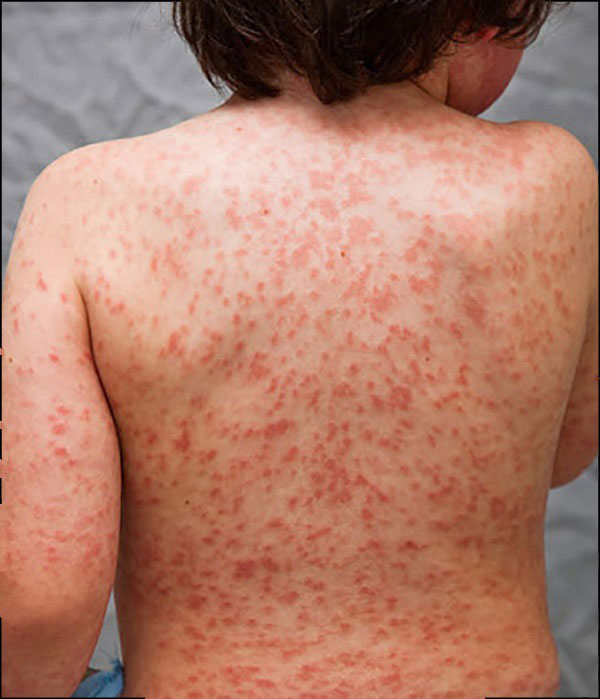
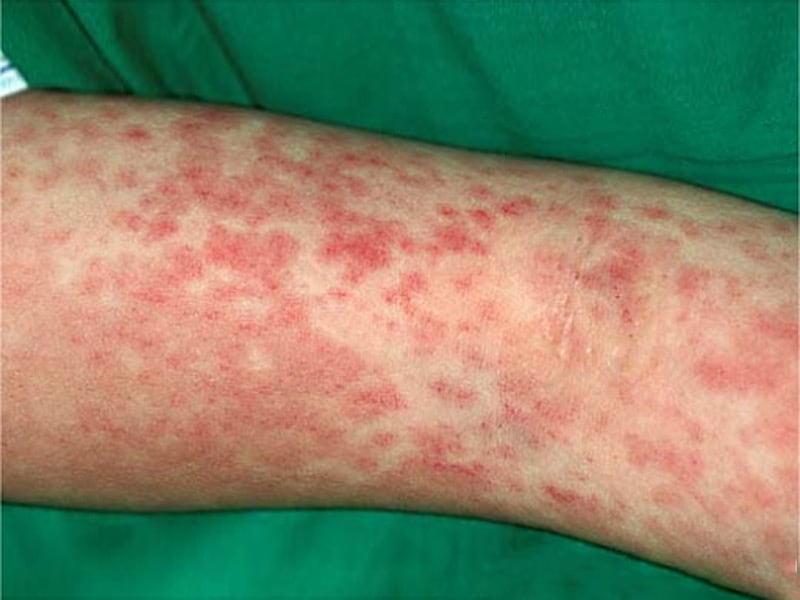
- A rash on the primary part of the body and in the genital region
- Red, dry, cracked lips and an extremely red, inflamed tongue
- Inflamed, red skin on the palms of the hands and the soles of the feet
- Inflamed lymph nodes in the neck and perhaps elsewhere
- Irritability
2nd phase
In the second phase of the disease, your child might develop:
- Peeling of the skin on the hands and feet, particularly the tips of the fingers and toes, usually in big sheets
- Joint pain
- Diarrhea
- Vomiting
- Abdominal pain
3rd phase
In the third phase of the disease, signs, and symptoms gradually go away unless complications develop. It might be as long as eight weeks before energy levels seem normal again.
WHEN SHOULD YOU SEE A DOCTOR?
If your child has a fever that lasts more than 3 days, contact your child’s doctor or primary care physician. Also, see your child’s doctor or primary care physician if your child has a fever along with four or more of the following signs and symptoms:
- Redness in both eyes
- A very red, inflamed tongue
- Redness of the palms or soles
- Skin peeling
- A rash
- Inflamed lymph nodes
Treating Kawasaki disease within ten days of when it started might greatly lower the chances of lasting damage.
KAWASAKI DISEASE CAUSES
No one knows what causes Kawasaki disease, but scientists do not believe the disease is contagious from person to person. A number of theories link the disease to bacteria, viruses, or other environmental factors, but nothing has been proven. Specific genes might make your child more likely to get Kawasaki disease.
KAWASAKI DISEASE RISK FACTORS
There are three things that could increase your child’s risk of developing Kawasaki disease
- Age – Children under five years old are most at risk of Kawasaki disease.
- Sex – Men are slightly more likely than women are to develop Kawasaki disease.
- Ethnicity – Children of Asian or Pacific Island origin, for example, Japanese or Korean, have higher rates of Kawasaki disease.
KAWASAKI DISEASE COMPLICATIONS
Kawasaki disease is a major cause of acquired heart disease among children. Although, with effective treatment, only a few children have lasting damage.
Heart complications include:
- Swelling of blood vessels, generally the coronary arteries, that supply blood to the heart
- Swelling of the heart muscle
- Heart valve problems
Any of these complications could affect your child’s heart. Swelling of the coronary arteries could lead to weakening and bulging of the artery wall (aneurysm). Aneurysms raise the risk of blood clots, which can lead to a heart attack or cause life-threatening internal bleeding.
For a very small percentage of children who develop coronary artery complications, Kawasaki disease could cause death, even with treatment.
KAWASAKI DISEASE DIAGNOSIS
There is no certain test available to diagnose Kawasaki disease. Diagnosis involves ruling out other diseases that cause identical signs and symptoms, including:
- Scarlet fever, which is caused by streptococcal bacteria and leads to fever, rash, chills, and sore throat
- Juvenile rheumatoid arthritis
- Stevens-Johnson syndrome, a disorder of the mucous membranes
- Toxic shock syndrome
- Measles
- Specific tick-borne diseases, for example, Rocky Mountain spotted fever
THE DOCTOR OR PRIMARY CARE PHYSICIAN WILL DO A PHYSICAL EXAM AND ORDER BLOOD AND URINE TESTS TO HELP IN THE DIAGNOSIS. TESTS MIGHT INCLUDE:
- Blood tests – Blood tests help rule out other illnesses and check your child’s blood cell count. A high white blood cell count and the presence of anemia and swelling are signs of Kawasaki disease. Testing for a substance known as B-type natriuretic peptide (BNP) that is released when the heart is under stress might be helpful in diagnosing Kawasaki disease. Although, more research is required to confirm this finding.
- Electrocardiogram – Electrodes are connected to the skin to measure the electrical impulses of your child’s heartbeat. Kawasaki disease could cause heart rhythm issues.
- Echocardiogram – This test uses ultrasound pictures to show how well the heart is working and could help identify issues with the coronary arteries.
KAWASAKI DISEASE TREATMENT
To lower the risk of complications, your child’s doctor or primary care physician will want to start treatment for Kawasaki disease as soon as possible, preferably while your child still has a fever. The goals of initial treatment are to reduce fever and swelling and prevent heart damage.
Treatment for Kawasaki disease might include:
- Gamma globulin – Infusion of an immune protein (gamma globulin) through a vein (intravenously) could reduce the risk of coronary artery issues.
- Aspirin – High doses of aspirin might help treat swelling. Aspirin could also decrease pain and joint inflammation, as well as lower the fever. Kawasaki treatment is a rare exception to the rule that says aspirin should not be given to children. Aspirin has been connected to Reye’s syndrome, a rare but potentially life-threatening condition, in children recovering from chickenpox or flu. Children should be given aspirin only under the supervision of a doctor or primary care physician.
Due to the risk of severe complications, early treatment for Kawasaki disease generally is given in a hospital.
AFTER THE INITIAL TREATMENT
Once the fever subsides, your child might require to take low-dose aspirin for at least 6 weeks and longer if he or she develops a coronary artery aneurysm. Aspirin helps stop clotting.
Although, if your child develops flu or chickenpox during treatment, he or she might require to prevent taking aspirin. Taking aspirin has been connected to Reye’s syndrome, a rare but potentially life-threatening condition that could affect the blood, liver, and brain of children and teenagers after a viral infection.
With treatment, your child might begin to improve soon after the first gamma globulin treatment. In the absence of treatment, Kawasaki disease lasts an average of twelve days. Although, heart complications might be longer-lasting.
MONITORING HEART ISSUES
If your child has any signs of heart issues, the doctor or primary care physician might suggest follow-up tests to check your child’s heart health at regular intervals, usually at six to eight weeks after the disease started, and then again after six months.
If heart problems continue, you might be referred to a doctor or primary care physician who specializes in treating heart disease in children (pediatric cardiologist). Treatment for heart complications associated with Kawasaki disease depends on what type of heart condition is present. If a coronary artery aneurysm ruptures, treatment might include anticoagulant drugs, stent placement, or bypass surgery.
Wait to vaccinate
If your child was given gamma globulin, it is a good idea to wait at least eleven months to get the chickenpox or measles vaccine, because gamma globulin could affect how well these vaccinations work.
If you or anyone you know is suffering from Kawasaki disease, our expert providers at Specialty Care Clinics will take care of your health and help you recover.
Call 469-545-9983 to book a telehealth appointment for an at home check-up.
