EYE MELANOMA – SYMPTOMS, CAUSES, AND TREATMENT
Melanoma is a type of cancer that forms in the cells that produce melanin — the pigment that gives your skin its color. Your eyes also have melanin-producing cells and could develop melanoma. Eye melanoma is otherwise known as ocular melanoma.
Most eye melanomas form in the part of the eye you cannot see when looking in a mirror. This makes eye melanoma hard to detect. In addition, eye melanoma generally does not cause early signs or symptoms.
Treatment is available for eye melanomas. Treatment for some small eye melanomas might not interfere with your vision. However, treatment for large eye melanomas generally causes some vision loss.
SYMPTOMS
Eye melanoma might not cause signs and symptoms. When they do happen, signs and symptoms of eye melanoma could include:
- A feeling of flashes or specks of dust in your vision (floaters)
- A growing dark spot on the iris
- A change in the shape of the dark circle (pupil) in the center of your eye
- Poor or blurry vision in one eye
- Loss of peripheral vision
WHEN SHOULD YOU SEE A DOCTOR?
Schedule an appointment with your doctor if you have any signs or symptoms that worry you. Unexpected changes in your vision signal an emergency, so seek immediate care in those situations.
CAUSES
It is unclear what causes eye melanoma.
Doctors know that eye melanoma happens when errors develop in the DNA of healthy eye cells. The DNA errors tell the cells to grow and multiply out of control so that mutated cells go on living when they would normally die. The mutated cells build up in the eye and form an eye melanoma.
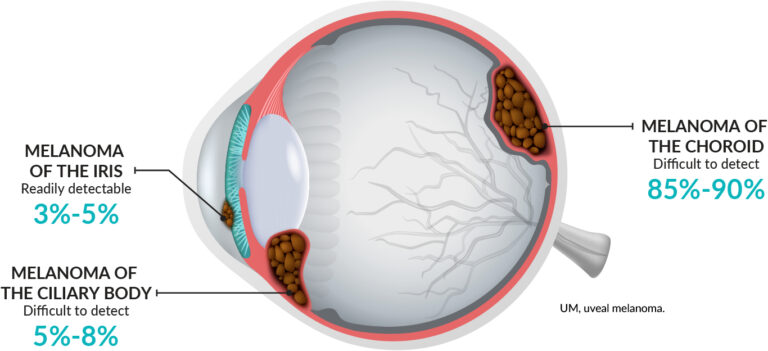
Where eye melanoma occurs
Eye melanoma most commonly forms in the cells of the middle layer of your eye (uvea). The uvea has three parts and each could be affected by eye melanoma:
- The iris, which is the colored part at the front of the eye.
- The choroid layer is the layer of blood vessels and connective tissue in between the sclera and the retina at the back of the uvea.
- The ciliary body, which is in the front of the uvea secretes the transparent liquid (aqueous humor) inside the eye.
Eye melanoma could also happen on the outermost layer on the front of the eye (conjunctiva), in the socket that encircles the eyeball, and on the eyelid, though these types of eye melanoma are very rare.
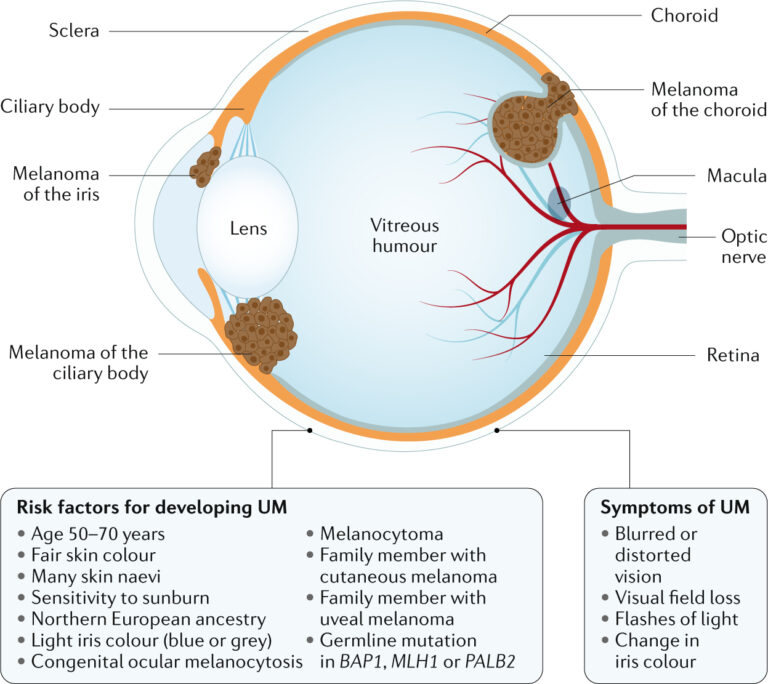
RISK FACTORS
Risk factors for primary melanoma of the eye include:
- Light eye color – People with blue eyes or green eyes have a higher risk of melanoma of the eye.
- Being white – White people have a higher risk of eye melanoma than do people of other races.
- Age – The risk of eye melanoma increases as you get older.
- Certain inherited skin disorders – The condition is known as dysplastic nevus syndrome, which causes abnormal moles, might increase your risk of developing melanoma on your skin and in your eye.
In addition to that, people with abnormal skin pigmentation involving the eyelids and adjacent tissues and increased pigmentation on their uvea — called ocular melanocytosis — also have an increased risk of developing eye melanoma. - Exposure to ultraviolet (UV) light – The role of ultraviolet exposure in eye melanoma is not clear. There is some evidence that exposure to UV light, like light from the sun or from tanning beds, might increase the risk of eye melanoma.
- Certain genetic mutations – Certain genes passed from parents to children might increase the risk of eye melanoma.
COMPLICATIONS
Complications of eye melanoma might include:
- Increasing pressure within the eye (glaucoma) – A growing eye melanoma might cause glaucoma. Signs and symptoms of glaucoma might include eye pain and redness, as well as blurry vision.
- Vision loss – Large eye melanomas usually cause vision loss in the affected eye and could cause complications, like retinal detachment, that also cause vision loss.
Small eye melanomas could cause some vision loss if they happen in critical parts of the eye. You might have difficulty seeing in the center of your vision or on the side. Very advanced eye melanomas could cause complete vision loss. - Eye melanoma that spreads beyond the eye – Eye melanoma could spread outside of the eye and to distant areas of the body, including the liver, lungs, and bones
DIAGNOSIS
To diagnose eye melanoma, your doctor may suggest:
- Eye exam – Your doctor will examine the outside of your eye, looking for enlarged blood vessels that could indicate a tumor inside your eye. Then, with the help of instruments, your doctor will look into your eye.
One method, known as binocular indirect ophthalmoscopy, uses lenses and a bright light mounted on your doctor’s forehead — a bit like a miner’s lamp. Another method, known as slit-lamp biomicroscopy, uses lenses and a microscope that produces an intense beam of light to illuminate the interior of your eye. - Eye ultrasound – An eye ultrasound uses high-frequency sound waves from a hand-held, wand-like apparatus known as a transducer to produce pictures of your eye. The transducer is positioned on your closed eyelid or on the front surface of your eye.
- Imaging of the blood vessels in and around the tumor (angiogram) – During an angiogram of your eye, a colored dye is administered into a vein in your arm. The dye travels to the blood vessels inside your eye.
A camera with special filters to detect the dye takes flash images every few seconds for several minutes. - Optical coherence tomography – The imaging test creates images of portions of the uveal tract and retina.
- Removing a sample of suspicious tissue for testing – In some cases, your doctor might recommend a procedure to remove a sample of tissue (biopsy) from your eye.
To remove the sample, a thin syringe is inserted into your eye and used to extract suspicious tissue. The tissue is tested in a lab to determine whether it contains eye melanoma cells.
An eye biopsy is not generally necessary to diagnose eye melanoma.
Determining whether cancer has spread
Your doctor might recommend additional tests and procedures to determine whether the melanoma has spread (metastasized) to other parts of your body. Tests might include:
- Blood tests to measure liver function
- Chest X-ray
- Computerized tomography (CT) scan
- Magnetic resonance imaging (MRI) scan
- Abdominal ultrasound
- Positron emission tomography (PET) scan
TREATMENT
Your eye melanoma treatment options will depend upon the location and size of the eye melanoma, as well as your overall health and your preferences.
Waiting to treat small eye melanomas
A small eye melanoma might not need immediate treatment. If the melanoma is small and is not growing, you and your doctor might choose to wait and watch for signs of growth.
If the melanoma grows or causes complications, you might choose to undergo treatment at that time.
Radiation therapy
Radiation therapy uses high-powered energy, like protons or gamma rays, to kill cancer cells. Radiation therapy is generally used for small to medium-sized eye melanomas.
The radiation is generally delivered to the tumor by placing a radioactive plaque on your eye, directly over the tumor in a procedure known as brachytherapy. The plaque is held in place with momentary stitches. The plaque looks similar to a bottle cap and contains many radioactive seeds. The plaque remains in place for 4 to 5 days before it is removed.
The radiation could also come from a machine that directs radiation, like proton beams, to your eye (external beam radiation, or teletherapy). This type of radiation therapy is usually administered over several days.
Laser treatment
Treatment that uses a laser to kill the melanoma cells might be an option in certain situations. One type of laser treatment, known as thermotherapy, uses an infrared laser and is sometimes used in combination with radiation therapy.
Photodynamic therapy
Photodynamic therapy combines medicines with a special wavelength of light. The medicine makes the cancer cells susceptible to light. The treatment affects the vessels and the cells that make up eye melanoma. Photodynamic therapy is used in smaller tumors, as it is not effective for larger cancers.
Cold treatments
Extreme cold (cryotherapy) might be used to destroy melanoma cells in some small eye melanomas, but this treatment is not commonly used.
Surgery
Operations used to treat eye melanoma include procedures to remove part of the eye or a procedure to remove the complete eye. What procedure you will undergo depends upon the size and location of your eye melanoma. Options might include:
- Surgery to remove the melanoma and a small area of healthy tissue – Surgery to remove the melanoma and a band of healthy tissue that surrounds it might be an option for treating small melanomas.
- Surgery to remove the entire eye (enucleation) – Enucleation is usually used for large eye tumors. It might also be used if the tumor is causing eye pain.
After the eye with melanoma is removed, an implant is inserted into the same position, and the muscles controlling the movement of the eye are connected to the implant, which enables the implant to move.
After you have had some time to heal, an artificial eye (prosthesis) is made. The front surface of your new eye will be custom painted to match your existing or current eye.
If you or anyone you know is suffering from eye melanoma, our expert providers at Specialty Care Clinics will take care of your health and help you recover.
Call us on (469) 545-9983 to book an appointment with our specialists.
