According to a new article published in Advanced Functional Materials, a medical team at Penn State University has begun testing the use of Bioprinting on rats to reduce the damage done by surgery. This means that there is a new method coming into place that may help remove scars and help prevent cosmetic damage to the skull or face from a neurosurgical operation.
WHAT IS BIOPRINTING?
It is similar to 3D printing, except bioprinting uses blueprints to create biomaterials such as organ-like-structures, cells, and more living cells and groupings. This “prints” living structures layer by layer onto other biocompatible materials like human skin, or that of another creature.
This means that it may be possible that after a surgical operation you will also undergo a bioprinting treatment. This would involve the doctors treating you noting what has been done to the area that may have damaged your skin, or other biomaterial. They will then use the bioprinter to recreate the area that has been damaged, rebuilding scar tissue with living cells to hide the damage.
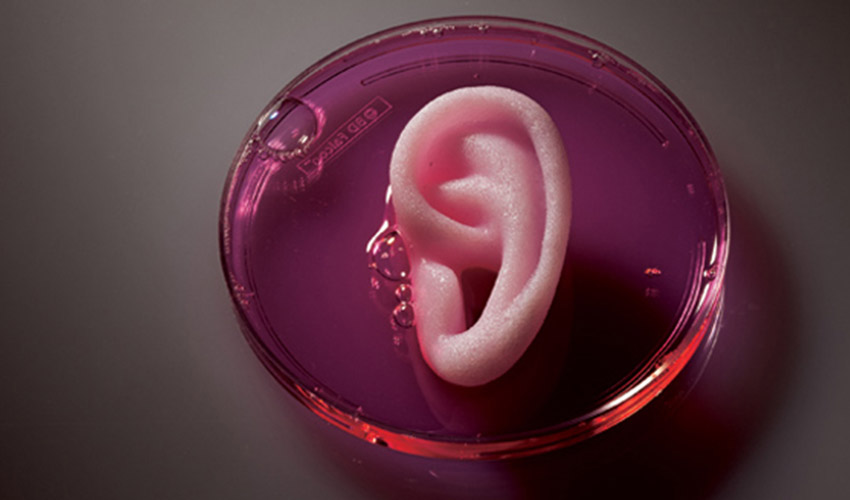
A Bioprinted Ear
WHY SHOULD YOU OPT FOR BIOPRINTING?
“Currently, fixing a hole in the skull involving both bone and soft tissue requires using bone from another part of the patient’s body or a cadaver. The bone must be covered by soft tissue with blood flow, also harvested from somewhere else, or the bone will die. Then surgeons need to repair the soft tissue and skin” (Moncal).
With the current technologies if there is extensive damage done to your tissue it is quite difficult to restore it to its original state as it takes multiple layers of reconstruction, which is very hard to take from concept to practice. Your bone and skin need different cells, or the area will die. With bioprinting this may be an issue that no longer gives surgery patients any worry as they know their scar will be healed with new invasive technology.
Ozbolat and his team had to lay the groundwork for using bioprinting to recover surgical wounds. This means they would need to lay a bone foundation for the bioprinting, and the skin layer at the same time. Previously, as noted, this was increasingly difficult because it took multiple layers of cells to be added, but with bioprinting this is done in one step. They tested the skull repair on rats who had 5mm holes in their head, and once this step was complete the team felt confident they could move to the epidermal layer.
“There is no surgical method for repairing soft and hard tissue at once,” said Ozbolat. “This is why we aimed to demonstrate a technology where we can reconstruct the whole defect — bone to epidermis — at once.”
RESULTS
The bone layer has been successfully tested that mimics periosteum, a vascularized tissue that covers the skull and surrounding bone. With over 50 tests done and a 100% success rate on the rats who had 6mm intrusions into their skulls, the team thinks they may have found “the next best thing” in surgical recovery and cosmetic prevention. Their work will soon raise questions on human surgical use, and the next trials may be on mammals with similar genetic and face structure to our own.
If you or anyone you know has suffered cosmetic damage (scars) as a result of neurosurgical operation, bioprinting may be the best option for you.
Call us today at 469-545-9983 to book an appointment with our expert neurosurgeons.
