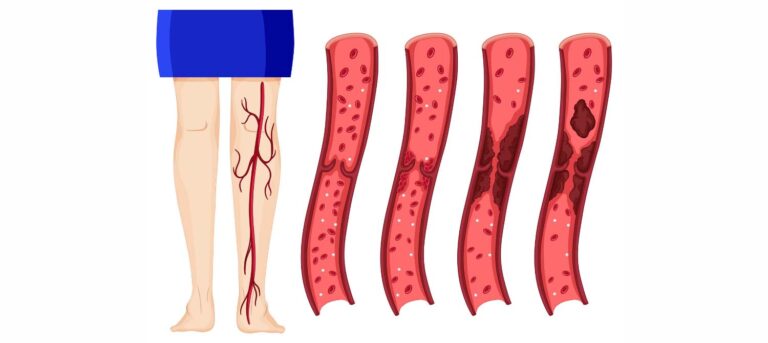
WHAT IS POPLITEAL VEIN THROMBOSIS?
The popliteal vein is one of the vital blood vessels in the lower body. It runs up the back of the knee and carries the blood from the lower leg to the heart. Sometimes, a blood clot, or a thrombosis, could block this vital vein. This is called deep vein thrombosis (DVT). It could restrict circulation in your legs. This could cause damage to your blood vessels and the surrounding tissue.
A clot could also break loose from the popliteal vein. It could then travel to the right side of the heart and then to the lungs, where it can cause numerous circulation and respiratory problems. A blood clot in your lungs is referred to as a pulmonary embolism (PE).
It is crucial to know how to avoid popliteal vein thrombosis and recognize the symptoms of this potentially life-threatening condition. If you are at high risk for popliteal vein thrombosis, you should learn more about its risks and how to keep the circulation in your legs as healthy as possible.
WHAT ARE THE SYMPTOMS?
The symptoms of a popliteal vein thrombosis involve pain, swelling, and tenderness around the area of the clot. While the vein is closer to the surface of the skin in the back of the knee, a clot could form anywhere in the blood vessel. The skin over the affected area might also feel warm to the touch.
The pain, which can begin in the lower leg, may feel like a cramp. That is why it is important to look for other symptoms like swelling. A typical muscle cramp will not result in swelling. If you notice that one leg is bigger than the other, get medical help promptly.
A blood clot in your circulatory system could cause a PE. If it gets to your brain, it could cause a stroke. If a clot is lodged in one of the arteries supplying blood to the heart muscle, the result could be a heart attack.
Frequently, a clot could exist without any obvious symptoms. This means you have to be aware of even small changes in the way you feel or the way your legs look.
If you experience breathing difficulties, it can mean that the clot has traveled to the lungs without you even knowing that it was in your vein.
You should always call 911 or your local emergency services if you are having difficulty breathing.
WHAT ARE THE CAUSES?
The two primary causes of popliteal vein thrombosis and other forms of DVT are damage to the vein and being bedridden or too sedentary.
Damage to your vein could occur due to :
- Smoking
- Drug use
- A major injury
- Chronic inflammation, which injures the internal lining of your vein
When your legs are still for long periods and you are not on your feet walking and moving around, blood flow in the legs gets sluggish. When blood is not circulating as it should, it could pool in a part of your vein and form a clot.
WHAT ARE THE RISK FACTORS?
If you have had a knee or hip replacement, or another major operation involving the legs, you are at an increased risk. This is partly because of being bedridden for a long operation and the recovery period that follows. Tissue from the bones or joints your surgeon is operating on could break off into tiny pieces. This could cause clots in your bloodstream.
Pregnancy could temporarily increase your risk of blood clots. Other risk factors associated with popliteal vein thrombosis include :
- People who smoke
- People who are obese
- Women who take birth control pills
- Women who take hormone replacement therapy
Factor V Leiden
Another risk factor is an inherited health condition known as factor V Leiden. It is a mutation of one of the proteins that help control bleeding and clotting. A mutation of the protein means you are at an increased risk for abnormal clots. You might have factor V Leiden and never experience clotting problems.
If you develop popliteal vein thrombosis or another form of DVT and you have a family history of clotting issues, your doctor might order a test for factor V Leiden. A blood test and a genetic test could help your doctor determine whether you have this inherited condition.
HOW IS A POPLITEAL VEIN THROMBOSIS DIAGNOSED?
Sudden onset of swelling, tenderness, and pain in the leg can indicate that you have a DVT. If the discomfort and swelling are in the area behind the knee, it might be a popliteal vein thrombosis.
Your doctor will do a physical examination. Following the exam, they might perform an ultrasound of your leg. The ultrasound will focus on the region of the suspected clot. If popliteal vein thrombosis is suspected, your doctor will give an ultrasound of your knee. An ultrasound uses sound waves to create a picture of the bones and tissue inside your leg.
They might also order venography. In this test, they administer a special dye into your vein and take an X-ray. The dye makes the picture inside the vein clearer and can reveal whether a blood clot is affecting your circulation.
A blood test known as a D-dimer test is also helpful. It tests your blood for a substance released through blood clots. Evidence of D-dimer in your blood suggests a vein thrombosis, but it does not help your doctor locate the clot. The other imaging tests and your physical symptoms will assist your doctor to locate it.
HOW IS A POPLITEAL VEIN THROMBOSIS TREATED?
If your doctor diagnoses you with a popliteal vein thrombosis, the first treatment you will receive is anticoagulant therapy. Anticoagulants are medicines that interfere with clotting. A few examples are heparin and warfarin (Coumadin, Jantoven).
Newer anticoagulants have been approved, involving rivaroxaban (Xarelto), apixaban (Eliquis), and dabigatran (Pradaxa). Anticoagulants and your body’s defenses might help a clot dissolve over time. The use of aspirin for a longer period might also help reduce the risk of new clots forming in your veins.
Depending on where the clot is located and how severe it is, your doctor may need to remove the clot. They could use special catheters to do this, but this is not always an option. Clots that are particularly difficult to reach may require surgery to remove.
Wearing compression stockings could also improve blood circulation in your lower legs.
WHAT IS THE OUTLOOK?
Having popliteal vein thrombosis is severe, but it can often be managed or treated if diagnosed in time. If you get treatment for it, there are not usually any long-term consequences. DVT tends to develop in people with advancing age, obesity, a history of smoking, or other circulation disorders, your doctor will have recommendations about how to avoid future clotting issues.
You might also have to stay on anticoagulant medication, also called a blood thinner, for the rest of your life. This can increase your risk of bleeding issues, but many people can take this medication without having problems with clotting or bleeding.
HOW CAN YOU PREVENT A POPLITEAL VEIN THROMBOSIS?
Because surgery and prolonged bed rest could lead to vein thrombosis, moving around as soon as possible after surgery is key to preventing popliteal vein thrombosis. You will need to follow your doctor’s advice and not risk hurting yourself after surgery, however.
Here are a few more ways to help prevent popliteal vein thrombosis and other forms of DVT :
- If you are sedentary during the day, try to move around more often. If you have difficulty walking, at least stand or move your legs from a seated position.
- Take medications, particularly anticoagulants, as prescribed.
- If you are at risk for DVT, your doctor may suggest you wear compression stockings on a regular basis. It might take time to get used to wearing them, but they could help save your life.
- If you smoke, try to quit as soon as you could. Ask your doctor for information on smoking cessation groups and treatments.
- If you are obese, talk with your doctor about strategies for weight loss.
- Do not skip your yearly physicals and regular doctor’s visits.
Preventing popliteal vein thrombosis is not always possible, but you could help prevent it if you take care of your health and follow these tips.
If you or anyone you know is suffering from popliteal vein thrombosis, our expert providers at Specialty Care Clinics will take care of your health and help you recover.
Call 469-545-9983 to book a telehealth appointment for an at-home check-up.