WHAT IS PHANTOM LIMB PAIN?
Phantom limb pain starts after the part of your arm or leg is amputated. You could feel pain in the limb that has been amputated. Phantom sensations and pain occur following amputation of different body parts like the eyes, teeth, tongue, nose, breast, penis, bowel, and bladder mostly due to limb amputation.
Phantom Limb pain may gradually go away. Some people after amputation have pain in the residual limb or remaining part of the limb.
The limb pain after amputation ranges from mild to severe that might last for seconds, hours, days or longer. It occurs after a medical amputation (removing part of a limb with surgery or after accidental amputation. Phantom pain can be managed with pain relievers and minor therapies.
Phantom limb pain is described as mild to agonizing pain which could be even disabling for some people. It may cause a lifelong battle with chronic pain. Women suffering from breast cancer who have had a breast removed might also feel phantom pain.

CAUSE OF PHANTOM LIMB PAIN
After the limb or any other body part amputation phantom pain may be caused this could be due to medical or psychological reasons. The exact reason for the phantom limb pain is not known to the researchers yet. As per the proposed hypothesis the sensations or pain is due to the brain’s attempt to reorganize signals to adjust to the changes in the body.
A person feels pain at the point of the missing body part in phantom pain. Other problems with amputated part of the body include:
- Phantom sensations: The missing limb feels like it is still part of the body. This is expressed as a sensation that a person experiences as phantom sensations (i.e. the person may forget that part of a lower limb is missing) and not pain. This is not due to medical reasons but due to psychological reasons.
- Phantom Pain : People experience actual pain that ranges from mild to severe in the amputated body part. Patients express feeling pressure, itching or even burning in the amputated limb.
- Residual limb pain: This pain is experienced in the remaining part of the limb (stump) left after the amputation occurred. Residual limb pain might be due to a medical reason like nerve damage or pressure on the nerve (entrapment). Approximately 7 in 10 people with limb loss are affected.
During the process of amputation, the peripheral nerves are detached. This causes disruption of tissue massively and neuronal injury leading to alteration of the normal pattern of afferent nerve input passing to the spinal cord.
This is followed by de-afferentation and the proximal portion of the detached nerve sprouts to form neuromas which enhance the sodium channel at the junction of amputation. This abnormal peripheral activity is the potential source of the stump pain and phantom pain.
Some of the factors that trigger the phantom limb pain are touch, urination or defecation, sexual intercourse, angina, cigarette smoking, changes in barometric pressure, herpes zoster and exposure to cold. People are often reluctant to share about the phantom limb pain with anyone for fear that they will be considered crazy but is it essential to share these pains at the start so the treatment can be started.
Doctors recommend localized anesthesia (spinal or epidural) during the hours or days leading up to amputation; this reduces the risk of developing phantom pain in people. This helps in reducing pain immediately after surgery and decreases the risk of lasting phantom limb pain.

SYMPTOMS OF PHANTOM LIMB PAIN
Phantom pain symptoms may be short-lived or last for days. Pain is usually described as shooting, stabbing, cramping, pins and needles, crushing, throbbing, or burning. The pain intensity and frequency usually decreases during the first 6 months after a limb loss. Some common symptoms apart from pain that people experience include:
- Burning sensation
- Itching or tingling
- Twisting
- Crushing
- Sensation like an electric shock
- Bone infection (osteomyelitis) or bone spurs
- Nerve damage (neuropathic pain) or inflammation (neuroma)
- Poor blood flow
- Poorly fitting prosthetic device
- Pressure injuries causing bedsores
- Skin or wound infections
- Stages of Lung Cancer
DIAGNOSIS OF PHANTOM LIMB PAIN
The healthcare provider will conduct a physical examination of the amputated part and prescribe tests to rule out the underlying causes of residual limb pain such as infection. The tests include blood tests and imaging scans like ultrasounds, MRI or CT scans.
Describing your pain precisely would help the doctor understand the underlying cause. Phantom pain and residual limb pain are common to occur at the same time but the treatments for these two problems are different. Thus, an accurate diagnosis is important for the treatment.
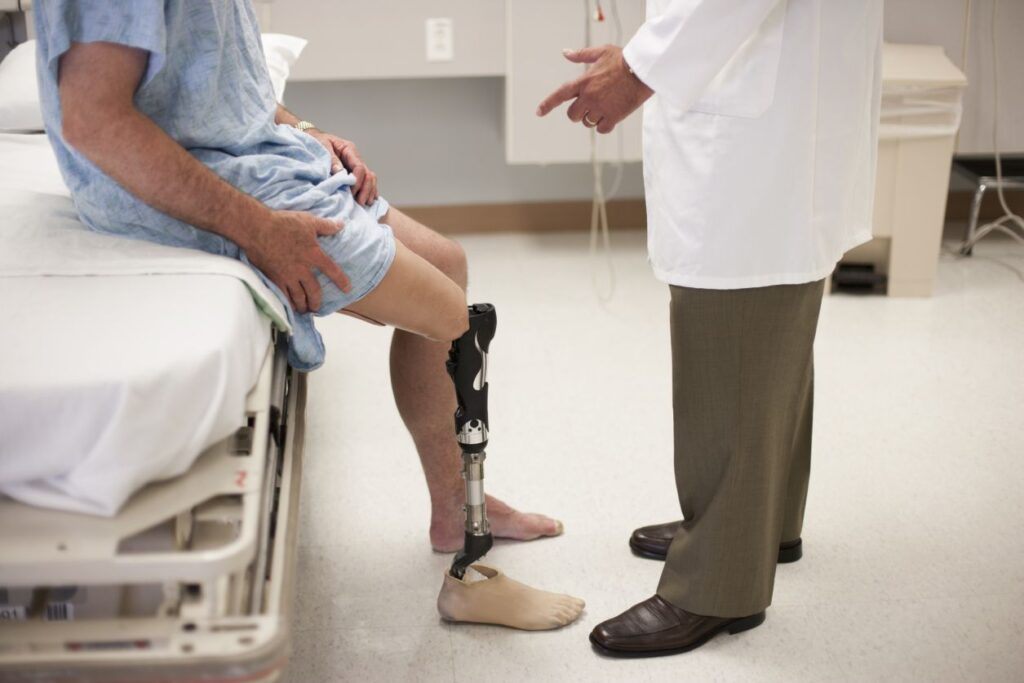
TREATMENT OF PHANTOM LIMB PAIN
Determining a treatment to relieve the phantom pain could be difficult. Doctors begin with medications to treat the symptoms and may add noninvasive therapies like acupuncture. A single drug would not be for everyone as well as not everyone benefitting from medications alone. Invasive options like injections or implanted devices are used when the non-invasive therapies do not provide relief. Surgery is recommended as a last resort.
MEDICATION
No specific medicine exists for phantom pain. However, some drugs are designed to treat other conditions that are helpful in relieving nerve pain.
- Over-the-counter (OTC) pain killer – Medicine available with prescription like Acetaminophen (Tylenol, others), ibuprofen (Advil, Motrin IB, others) or naproxen sodium (Aleve) help relieve pain.
- Antidepressants – They help relieve pain caused by damaged nerves. Commonly used tricyclic antidepressants are amitriptyline, nortriptyline (Pamelor) and tramadol (Conzip, Ultram).
- Anticonvulsants – These also provide relief in nerve pain at the site of amputation. Example, gabapentin (Gralise, Neurontin) and pregabalin (Lyrica).
- N-methyl-d-aspartate (NMDA) receptor antagonists – These anesthetics work by binding to the NMDA receptors on the nerve cells in the brain. These help in blocking the activity of glutamate, which is a protein playing an important role in relaying nerve signals.
- Narcotics – For severe pain narcotics or opioids like codeine and morphine are used.
MEDICAL THERAPIES
Along with medication non-invasive therapies help in treatment of phantom pain
- Mirror box – The patient would watch the process in a mirror while receiving physical therapy that helps to re-map the brain’s neural pathways for registering the limb is no longer present. Patient would feel the imaginary movement of the amputated limb behaving as the normal movement of the through a mirror. This therapy is proven efficient for patients with post-amputation pain.
- Repetitive transcranial magnetic stimulation (rTMS) – This therapy involves an electromagnetic coil placed against the forehead sending short pulses that are sent through the coil. This induces small electrical currents in the nerves which are located in a specifically targeted area of the brain. This helps in rewiring the brain signals and eases off the pain.
- Spinal cord stimulation – The therapy involves insertion of tiny electrodes along the spinal cord. A small amount of electrical current provided continuously to the spinal cord helps in relieving pain.
PREGNANCY
A healthy pregnancy is possible in women who have Takayasu’s arteritis. But the disease and drugs used to treat it could affect your fertility and pregnancy. If you have Takayasu’s arteritis and are planning on becoming pregnant, work with your doctor or primary care physician to develop a plan to limit complications of pregnancy before you conceive. See your doctor or primary care physician regularly during your pregnancy for check-ups.
TAKAYASU’S ARTERITIS DIAGNOSIS
Your doctor or primary care physician will ask you about your signs and symptoms, perform a physical examination, and take your medical history. He or she might also have you undergo some of the following tests and procedures to help rule out other conditions that resemble Takayasu’s arteritis and to confirm the diagnosis. Some of these tests might also be used to check on your progress during treatment.
- Blood tests – These tests could be used to look for signs of inflammation. Your doctor or primary care physician might also check for anemia.
- X-rays of your blood vessels (angiography) – During an angiogram, a long, flexible tube (catheter) is inserted into a big artery or vein. A special contrast dye is then administered into the catheter, and X-rays are taken as the dye fills your arteries or veins.
- The resulting pictures allow your doctor or primary care physician to see if blood is flowing normally or if it is being slowed or interrupted due to narrowing (stenosis) of a blood vessel. A person with Takayasu’s arteritis usually has several regions of stenosis.
- Magnetic resonance angiography (MRA) – This less invasive form of angiography produces detailed pictures of your blood vessels without the use of catheters or X-rays. Magnetic resonance angiography (MRA) works by using radio waves in a strong magnetic field to produce data that a computer turns into detailed pictures of tissue slices. During this test, a contrast dye is administered into a vein or artery to help your doctor or primary care physician better see and examine the blood vessels.
- Computerized tomography (CT) angiography – This is another non-invasive form of angiography combining computerized analysis of X-ray pictures with the use of intravenous contrast dye to allow your doctor or primary care physician to check the structure of your aorta and its nearby branches and to monitor blood flow.
- Ultrasonography – Doppler ultrasound, a more sophisticated version of the common ultrasound, has the ability to produce very high-resolution pictures of the walls of specific arteries, like those in the neck and shoulder. It might be able to detect subtle changes in these arteries before other imaging techniques could.
- Positron emission tomography (PET) – This imaging test is usually done in combination with computerized tomography (CT) or magnetic resonance imaging (MRI). Positron emission tomography (PET) could measure the intensity of inflammation in blood vessels. Before the scan, a radioactive drug is administered into a vein or an artery to make it easier for your doctor or primary care physician to see areas of reduced blood flow.
SURGERY
Deep brain stimulation and motor cortex stimulation involves the current to be delivered within the brain. This involves magnetic resonance imaging (MRI) scan to position the electrodes correctly thereby helping in relieving pain.
OUTLOOK
Learning to live without a limb is challenging especially with phantom pain. This could be accompanied with depression and anxiety. Support of family and loved ones help in coping up with the condition.
If you or anyone you know is suffering from phantom limb pain, our expert providers at Specialty Care Clinics will take care of your health and help you recover.
Call us on 469-545-9983 to book an appointment with Dr. Rao Kamran Ali.
