Chilblains or pernio is a common skin disorder resulting from exposure to cold usually just above freezing, and recurrent trauma. Cold exposure or trauma causes inflammation along with erythematous lesions on the feet, hands, underlying medical conditions, or face (less commonly) that are precipitated by rapid rewarming after exposure to cold and humidity.
This has been reported as one of the most common cutaneous manifestations associated with COVID-19. This has previously been associated with vasospasm and a type I interferon response.
Chilblains occur commonly in temperate climates. Women and children are more sensitive towards chilblains. Chilblains or pernio occur as small itchy, red, or sometimes blue to purple swellings on the skin that can be painful. Reaction to severe cold weather causes our capillaries to shrink. This helps to maintain the warmth of blood close to our body and not close to the skin where heat is lost. If we rewarm the feet too quickly it can lead to leakage of fluid and blood into the toes leading to chilblains. The redness is caused by the fluid and blood in the tissue. This can lead to irritation and itching, which can sometimes break down to become a small ulcer prone to infection.
The best way to avoid chilblain is by limiting your exposure to cold, dressing warmly, and covering exposed skin.
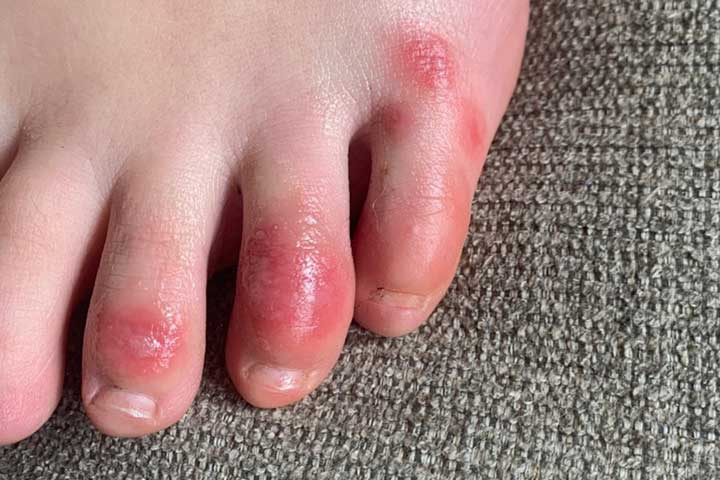
CAUSE OF CHILBLAINS
The blood vessels become narrow when exposed to extremely cold temperatures. After returning to warmth, the blood vessels would expand again. The tiny blood vessels present under the skin constrict when subjected to cold temperature. As the blood vessels become narrow the supply of blood may become very slow. Sometimes, this change in sudden temperature would result in blood leaking out of the blood vessels, causing inflammation and chilblain symptoms. The symptoms are severe if the change from cold to warmth is abrupt.
Cold weather usually causes small blood vessels near the surface of your skin to tighten. Abruptly warming up these small vessels forces them to expand quickly. The sudden expansion of the blood vessels causes them to leak into nearby tissue, resulting in swelling. Inflammation causes irritation of the nerves in the affected area, causing pain.
The rate of temperature change may play an important part. Some people get chilblains even when they warm up cold skin too quickly.
Chilblains can affect people of any age but elderly people are at high risk. Women and children are more susceptible to chilblains. People with sensitive skin are more susceptible to getting chilblains when exposed to cold, including:
- People suffering from circulation problems.
- People suffering from lupus.
- People living in draughty and cold.
- People whose homes are not well insulated.
- Tobacco smokers.
- Underweight individuals.
- People suffering from Raynaud’s disease.
Chilblains if not treated on time might lead to:
- Infections
- Skin ulcers
- Scarring
Complications may arise if you are suffering from an underlying medical condition such as diabetes or COVID-19 infection.
In severe cases, there can be a permanent discoloration of the affected area. To avoid any complications you should not scratch or rub the affected area.
SYMPTOMS OF CHILBLAINS
COVID-19 is associated with various cutaneous manifestations, such as chilblain. People experience eruption on the feet referred to as “COVID toes.” These symptoms are common among younger patients. The reason behind these lesions in COVID-19 patients is unknown.
Chilblains mostly appear a short while after being exposed to the cold temperature or trauma. Symptoms might worsen if the individual walks into somewhere warm or quickly warms the feet.
Initially, only one chilblain occur leading to developing several of them. Eventually, they may join together to form a larger swollen, red area of skin.
Chilblains signs and symptoms include:
- Burning and itching sensation in feet or toes
- The color of the affected area of skin may change from red to dark blue.
- The skin of the affected area may become inflamed or swollen.
- Sores and blisters may rarely appear.
Usually, chilblains do not cause any complications and vanish in time without a trace. But, sometimes, if not treated on time it can cause complications such as:
- An infection may develop in the affected area of the skin. Infection may occur or worsen if you scratch it allowing the germs to manifest.
- Blisters may occur over the skin affected with a chilblain. This would delay the healing process.
- Rarely, the skin breaks down to leave a small ulcer making it prone to infection.
- In certain cases, chilblains can become persistent or chronic, especially in people with repeated exposure to cold conditions. The skin does not get the time to heal and becomes scarred over time. The skin color may change permanently.

DIAGNOSIS OF CHILBLAINS
The podiatrist can diagnose chilblains during a basic physical examination with their appearance. They would enquire about any recent exposure to unusually cold or wet weather. Rarely, they may decide to do a biopsy of the affected area to rule out cancer. A biopsy involves removing a small tissue and check for signs of cancer under a microscope, such as skin cancer.
The podiatrist would rule out any potentially related conditions, such as lupus, Raynaud’s phenomenon, erythromelalgia, ischemia, or a circulation issue, that require treatment.
TREATMENT OF CHILBLAINS
Chilblains can be easily treated at home if they are at an initial stage. Some home treatments that are beneficial include:
- Resist the urge to scratch and itch, as this may further damage the skin.
- Calamine lotion or witch hazel help to soothe the itching.
- Use deep heat or similar heating methods on the feet to promote warmth and circulation.
- Wear woolen or cotton socks to keep the affected area warm
- Keep your whole body warm.
- Do not massage, rub, or apply direct heat.
The podiatrist would recommend cream and gels to treat the related symptoms such as:
- Corticosteroid cream: This may help in reducing inflammation and itching. These are available over-the-counter or online.
- Vasodilators: In severe cases, vasodilators such as nifedipine or diltiazem are prescribed. Vitamin D and calcium supplements help ease symptoms such as redness and itching in the affected area.
Therapy such as Low-Level Laser Therapy help in the treatment of chilblains by warming the affected area.
PREVENTION OF CHILBLAINS
Prevention is the key to chilblains. You can follow the below tips to avoid chilblains occurring to you:
- Keeping your feet warm always, especially in cold temperatures.
- Avoid warming your feet too quickly.
- If your feet are cold warm them up slowly.
- Avoid using a hot shower or keeping your feet in front of the heater immediately after coming from the cold.
- Increase the temperature slowly and gradually to warm your feet after coming from cold.
- Wear a pair of slippers or thick woolen socks that slowly warm your feet.
- Avoid walking barefoot in cold.
- Side-effects to certain medicines may constrict tiny blood vessels making you susceptible to chilblains.
TAKEAWAY
Chilblains usually recover in one to three weeks after cold exposure. People suffering from chilblains mostly don’t need to see a doctor. But, if you’re in pain or have an infection, see a podiatrist. The podiatrist may suggest treatment for chilblain or refer you to a skin specialist or cardiologist.
