WHAT IS THROMBOPHLEBITIS?
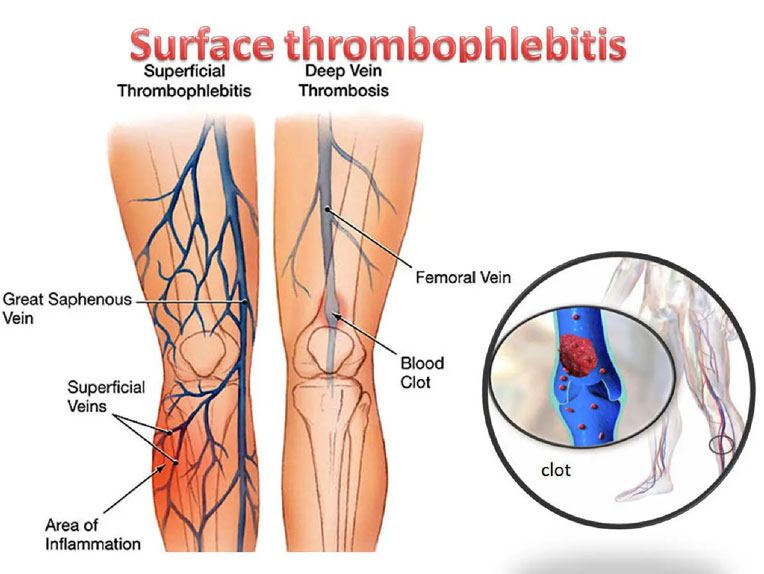
Thrombophlebitis is an inflammatory process that causes a blood clot to form and block one or more veins, generally in the legs. The affected vein may be near the surface of the skin (superficial thrombophlebitis) or deep within a muscle (deep vein thrombosis, or DVT).
The causes of thrombophlebitis involve trauma, surgery, or prolonged inactivity.
DVT increases the risk of severe health problems. It is generally treated with blood-thinning medications. Superficial thrombophlebitis is at times treated with blood-thinning medications, too.
SYMPTOMS
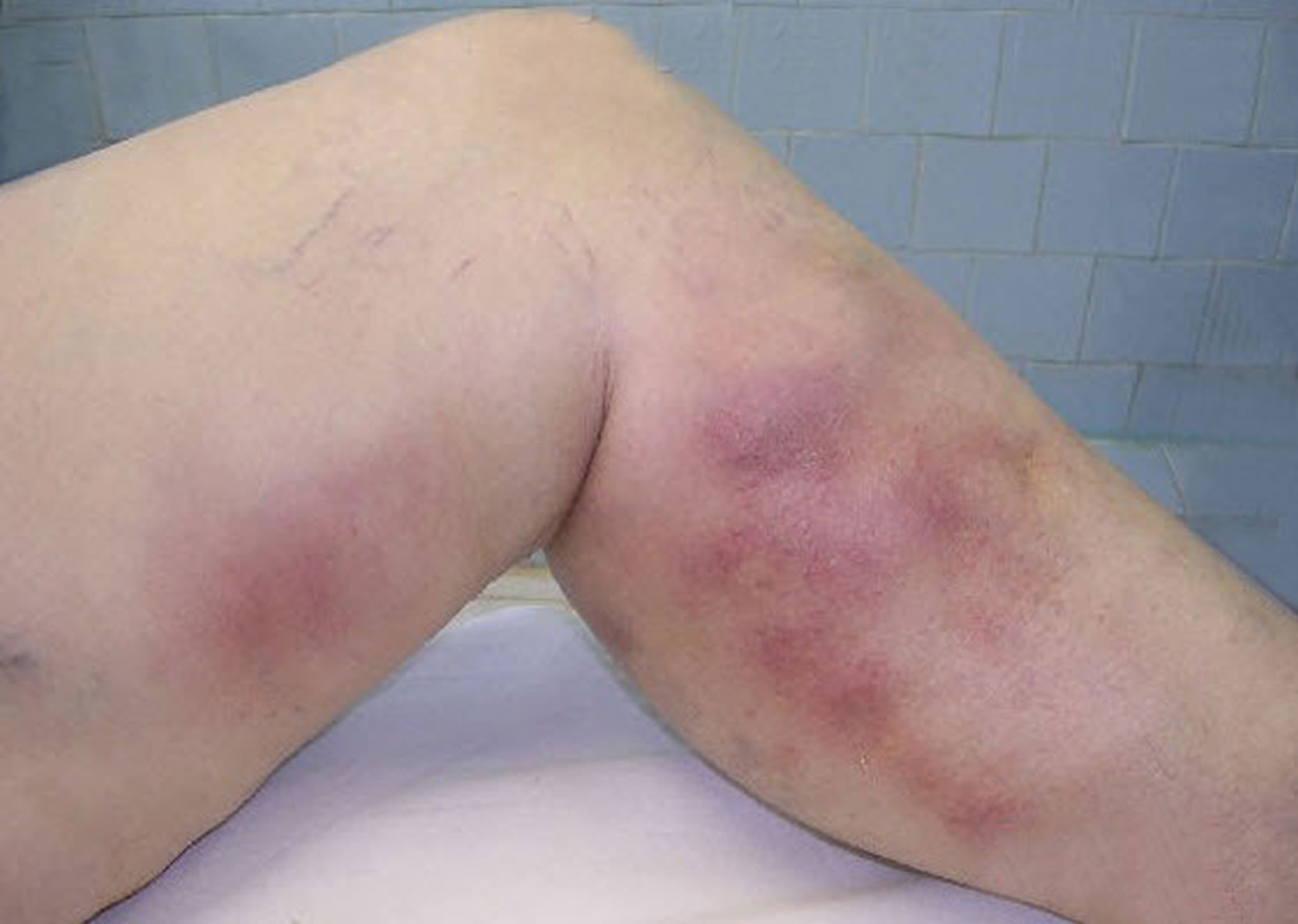
Superficial thrombophlebitis signs and symptoms include:
- Warmth, tenderness, and pain in the affected region
- Redness and swelling
Deep vein thrombosis signs and symptoms include:
- Pain
- Swelling
When a vein close to the surface of the skin is affected, you may see a red, hard cord just under the surface of the skin that is tender to the touch. When a deep vein in the leg is affected, the leg might become swollen, tender, and painful.
WHEN SHOULD YOU SEE A DOCTOR?
See your doctor right away if you have a red, swollen, or tender vein — particularly if you have one or more risk factors for thrombophlebitis.
Call 911 or your local emergency number if:
- The vein swelling and pain are serious
- You also have shortness of breath or chest pain, are coughing up blood, or have other symptoms that might indicate a blood clot traveling to your lungs (pulmonary embolism)
Have someone take you to your doctor or emergency room, when possible. It may be difficult for you to drive, and it is helpful to have someone with you to help you remember the information you receive.
CAUSES
The cause of thrombophlebitis is a blood clot, which could form in your blood as a result of:
- An injury to a vein
- An inherited blood-clotting disorder
- Being immobile for long periods, like during an injury or a hospital stay
RISK FACTORS
Your risk of thrombophlebitis may increase if you:
- Are inactive for a prolonged period, either because you are confined to bed or you are traveling in a car or plane for a long period
- Have varicose veins, which are a frequent cause of superficial thrombophlebitis
- Have a pacemaker or have a thin, flexible tube (catheter) in a central vein, for treatment of a medical condition, which might irritate the blood vessel wall and reduce blood flow
- Are pregnant or have just given birth
- Use birth control pills or hormone replacement therapy, which could make your blood more likely to clot
- Have a family history of a blood-clotting disorder and a tendency to form blood clots
- Have had previous episodes of thrombophlebitis
- Have had a stroke
- Are older than 60
- Are overweight or obese
- Have cancer
- Smoke
If you have one or more risk factors, discuss prevention strategies with your doctor before taking long flights or road trips, or if you are planning to have elective surgery, recovery from which will need you not to move much.
COMPLICATIONS
Complications from superficial thrombophlebitis are uncommon. However, if you develop DVT, the risk of severe complications increases. Complications may include:
- Blood clot in the lungs (pulmonary embolism) – If part of a deep vein clot becomes dislodged, it could travel to your lungs, where it could block an artery (embolism) and become potentially life-threatening.
- Lasting leg pain and swelling (post-phlebetic syndrome) – This condition, also known as post-thrombotic syndrome, could develop months or years after you have had DVT. The pain could be disabling.
PREVENTION
Sitting during a long flight or car ride can cause your ankles and calves to swell up and increases your risk of thrombophlebitis. To help prevent a blood clot:
- Take a walk – If you are flying or riding a train or bus, walk up, and down the aisle once an hour or so. If you are driving, stop every hour or so and move around.
- Move your legs regularly – Flex your ankles, or carefully press your feet against the floor or footrest in front of you at least ten times each hour.
- Drink plenty of water or other non-alcoholic fluids to stay away from dehydration.
DIAGNOSIS
To diagnose thrombophlebitis, your doctor will ask you about your discomfort and search for affected veins near your skin’s surface. To determine whether you have superficial thrombophlebitis or deep vein thrombosis, your doctor may choose one of these tests:
- Ultrasound – A wand-like device (transducer) moved over the affected region of your leg sends sound waves into your leg. As the sound waves travel through your leg tissue and reflect back, a computer transforms the waves into a moving picture on a video screen.
This test could confirm the diagnosis and distinguish between superficial and deep vein thrombosis. - Blood test – Almost everyone with a blood clot has an elevated blood level of a naturally occurring, clot-dissolving substance known as D dimer. But D dimer levels could be elevated in other conditions. So a test for D dimer is not conclusive but could indicate the need for further testing.
It is also useful for ruling out DVT and for identifying people at risk of developing thrombophlebitis repeatedly.
TREATMENT
For superficial thrombophlebitis, your doctor may recommend applying heat to the painful area, elevating the affected leg, using an over-the-counter nonsteroidal anti-inflammatory drug (NSAID) and possibly wearing compression stockings. The condition generally gets better on its own.
Your doctor may also recommend these treatments for both types of thrombophlebitis:
- Blood-thinning medications – If you have deep vein thrombosis, an injection of a blood-thinning (anticoagulant) medication, like low molecular weight heparin, fondaparinux (Arixtra), or apixaban (Eliquis), could help prevent clots from growing bigger. After the first treatment, you will likely be told to take warfarin (Jantoven) or rivaroxaban (Xarelto) for several months to keep preventing clot growth. Blood thinners could cause excessive bleeding. Always follow your doctor’s instructions with care.
- Clot-dissolving medications – Treatment with a clot-dissolving drug is known as thrombolysis. The medication alteplase (Activase) is used to dissolve blood clots in people with extensive DVT, including those with a blood clot in the lungs (pulmonary embolism).
- Compression stockings – Prescription-strength compression stockings help prevent swelling and decrease the chances of complications of DVT.
- Vena cava filter – If you cannot take blood thinners, a filter might be inserted into the main vein in your abdomen (vena cava) to prevent clots that break loose in your leg veins from lodging in your lungs. Usually, the filter is removed when it is no longer required.
- Varicose vein stripping – A surgeon could remove varicose veins that cause pain or recurrent thrombophlebitis. The procedure includes removing a long vein through small incisions. Removing the vein would not affect blood flow in your leg because veins deeper in the leg take care of the increased volumes of blood.
If you or anyone you know is suffering from thrombophlebitis, our expert providers at Specialty Care Clinics will take care of your health and help you recover.
Call 469-545-9983 to book a telehealth appointment or an at-home check-up.