WHAT IS MYOCARDIAL ISCHEMIA?
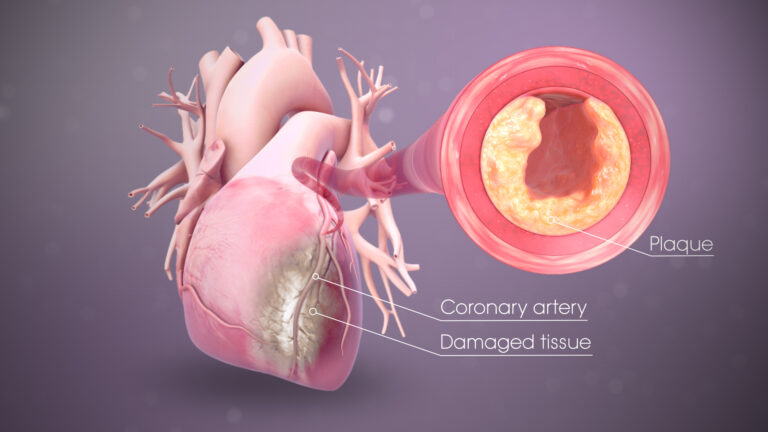
Myocardial ischemia happens when blood flow to your heart is decreased, preventing the heart muscle from receiving enough oxygen. The decreased blood flow is generally the result of a partial or full obstruction of your heart’s arteries (coronary arteries).
Myocardial ischemia, also known as cardiac ischemia, decreases the heart muscle’s ability to pump blood. An unexpected, severe blockage of one of the heart’s arteries could lead to a heart attack. Myocardial ischemia may also cause severe abnormal heart rhythms.
Treatment for myocardial ischemia includes improving blood flow to the heart muscle. Treatment might include medications, a procedure to open blocked arteries (angioplasty), or bypass surgery.
Choosing heart-healthy lifestyle choices is crucial in treating and preventing myocardial ischemia.
MYOCARDIAL ISCHEMIA SYMPTOMS
Some people who have myocardial ischemia do not have any signs or symptoms (silent ischemia).
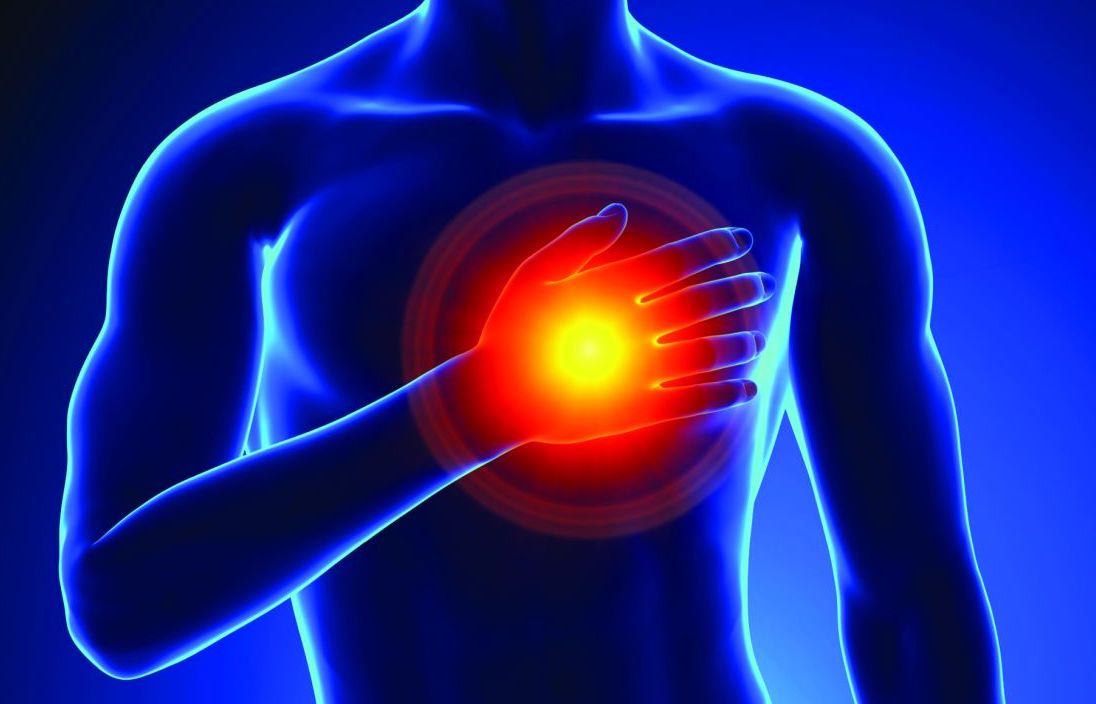
When they do happen, the most common is chest pressure or pain, commonly on the left side of the body (angina pectoris). Other signs and symptoms — which may be experienced more commonly by women, older people, and people with diabetes — include:
- Neck or jaw pain
- Shoulder or arm pain
- A fast heartbeat
- Shortness of breath during physical activity
- Nausea and vomiting
- Sweating
- Fatigue
- Cardiac Ischemia
WHEN SHOULD YOU SEE A DOCTOR?
Get emergency help if you have severe chest pain or chest pain that does not go away.
MYOCARDIAL ISCHEMIA CAUSES
Myocardial ischemia happens when the blood flow through one or more of your coronary arteries is reduced. The low blood flow reduces the amount of oxygen your heart muscle receives.
Myocardial ischemia could develop gradually as arteries become blocked over time. Or it could happen quickly when an artery becomes blocked suddenly.
Conditions that could cause myocardial ischemia include:
Coronary artery disease (atherosclerosis) – Plaques made up mostly of cholesterol accumulate on your artery walls and reduce blood flow. Atherosclerosis is the most prevalent cause of myocardial ischemia.
Blood clot – The plaques that develop in atherosclerosis could rupture, causing a blood clot. The clot may block an artery and lead to unexpected, severe myocardial ischemia, resulting in a heart attack. Rarely, a blood clot may travel to the coronary artery from elsewhere in the body.
Coronary artery spasm – This temporary tightening of the muscles in the artery wall could briefly reduce or even prevent blood flow to part of the heart muscle. Coronary artery spasm is an unusual cause of myocardial ischemia.
Myocardial Ischemia
Chest pain related to myocardial ischemia could be triggered by:
- Physical exertion
- Emotional stress
- Cold temperatures
- Cocaine use
- Eating a heavy or large meal
- Sexual intercourse
MYOCARDIAL ISCHEMIA RISK FACTORS
Factors that could increase your risk of developing myocardial ischemia include:
- Tobacco – Smoking and long-term exposure to second-hand smoke could damage the inside walls of arteries. The damage could let deposits of cholesterol and other substances accumulate and slow blood flow into the coronary arteries. Smoking causes the coronary arteries to spasm and might also increase the risk of blood clots.
- Diabetes – Type 1 and type 2 diabetes are connected to an increased risk of myocardial ischemia, heart attack, and other heart issues.
- High blood pressure – Over time, high blood pressure could speed up atherosclerosis, causing damage to the coronary arteries.
- High blood cholesterol level – Cholesterol is a major part of the deposits that could narrow your coronary arteries. A high level of “bad” (low-density lipoprotein, or LDL) cholesterol in your blood might be due to an inherited condition or a diet high in saturated fats and cholesterol.
- High blood triglyceride level – Triglycerides, another type of blood fat, also might contribute to atherosclerosis.
- Obesity – Obesity is related to diabetes, high blood pressure, and high blood cholesterol levels.
- Waist circumference – A waist measurement of more than 35 inches (89 centimeters) for women and 40 inches (102 cm) for men raises the risk of high blood pressure, diabetes, and heart disease.
- Lack of physical activity – Not getting enough exercise contributes to obesity and is connected to higher cholesterol and triglyceride levels. People who get regular aerobic exercise have better heart health, which is related to a reduced risk of myocardial ischemia and heart attack. Exercise also decreases blood pressure.
MYOCARDIAL ISCHEMIA COMPLICATIONS
Myocardial ischemia could lead to severe complications, including:
- Heart attack – If a coronary artery becomes completely obstructed, the lack of blood and oxygen could result in a heart attack that destroys a portion of the heart muscle. The damage could be severe and sometimes fatal.
Irregular heart rhythm (arrhythmia) – An abnormal heart rhythm could weaken your heart and might be life-threatening. - Heart failure – Over time, repeated episodes of ischemia might lead to heart failure.
MYOCARDIAL ISCHEMIA PREVENTION
Similar lifestyle habits that could help treat myocardial ischemia could also help prevent it from developing in the first place. Leading a heart-healthy lifestyle could help keep your arteries strong, elastic and smooth, and permit for maximum blood flow.
MYOCARDIAL ISCHEMIA DIAGNOSIS
Your doctor will start by asking questions about your medical history and with a physical examination. After that, your doctor may recommend:
- Electrocardiogram (ECG) – Electrodes connected to your skin record the electrical activity of your heart. Specific changes in your heart’s electrical activity might be a sign of heart damage.
- Stress test – Your heart rhythm, blood pressure, and breathing are tracked while you walk on a treadmill or ride a stationary bike. Exercise makes your heart pump harder and faster than usual, so a stress test could identify heart problems that may not be noticeable otherwise.
- Echocardiogram – Sound waves directed at your heart from a wand-like device placed on your chest generate video pictures of your heart. An echocardiogram could help identify whether a region of your heart has been damaged and is not pumping normally.
- Stress echocardiogram – A stress echocardiogram is identical to a regular echocardiogram, except the test is done after you exercise in the doctor’s office on a treadmill or stationary bike.
- Nuclear stress test – Small amounts of radioactive material are administered into your bloodstream. While you exercise, your doctor could watch as it flows through your heart and lungs — allowing blood-flow problems to be detected.
- Coronary angiography – A dye is administered into the blood vessels of your heart. Then a series of X-ray pictures (angiograms) are taken, showing the dye’s path. This test allows your doctor a detailed look at the inside of your blood vessels.
- Cardiac Computed Tomography (CT) scan – This test could determine if you have an accumulation of calcium in your coronary arteries — a sign of coronary atherosclerosis. The heart arteries could also be seen using computed tomography (CT) scanning (coronary CT angiogram).
MYOCARDIAL ISCHEMIA TREATMENT
The aim of myocardial ischemia treatment is to improve blood flow to the heart muscle. Depending upon the severity of your condition, your doctor might recommend medications, surgery, or both.
Medications
Medications to treat myocardial ischemia include:
- Aspirin – A daily aspirin or other blood thinners could lower your risk of blood clots, which may help prevent blockage of your coronary arteries. Ask your doctor before starting to take aspirin because it may not be appropriate if you have a bleeding disorder or if you are already taking another blood thinner.
- Nitrates – These medications broaden arteries, improving blood flow to and from your heart. Better blood flow means your heart does not have to work as hard.
- Beta-blockers – These medications help relax your heart muscle, slow your heartbeat and reduce blood pressure so blood could flow to your heart more easily.
- Calcium channel blockers – These medications relax and broaden blood vessels, increasing blood flow in your heart. Calcium channel blockers also slow your pulse and decrease the workload on your heart.
- Cholesterol- lowering medications – These medications reduce the primary material that deposits on the coronary arteries.
- Angiotensin- converting enzyme (ACE) inhibitors – These medications help relax blood vessels and reduce blood pressure. Your doctor may recommend an angiotensin-converting enzyme (ACE) inhibitor if you have high blood pressure or diabetes in addition to myocardial ischemia. Angiotensin- converting enzyme (ACE) inhibitors might also be used if you have heart failure or if your heart does not pump blood effectively.
- Ranolazine (Ranexa) – This medication helps relax your coronary arteries to relieve angina. Ranolazine might be prescribed with other angina medications, like calcium channel blockers, beta-blockers, or nitrates.
What is Myocardial Ischemia?
Procedures to improve blood flow
Sometimes, more aggressive treatment is required to improve blood flow. Procedures that might help include:
Angioplasty and stenting – A long, thin tube (catheter) is inserted into the narrowed portion of your artery. A wire with a small balloon is threaded into the narrowed region and inflated to widen the artery. A small wire mesh coil (stent) is generally inserted to keep the artery open.
Coronary artery bypass surgery – A surgeon uses a vessel from another part of your body to create a graft that permits blood to flow around the blocked or narrowed coronary artery. This type of open-heart surgery is generally used only for people who have several narrowed coronary arteries.
Enhanced external counterpulsation – This non-invasive outpatient treatment may be recommended if other treatments have not worked. Cuffs that have been wrapped around your legs are slightly inflated with air then deflated. The resulting pressure on your blood vessels could improve blood flow to the heart.
If you or anyone you know is suffering from myocardial ischemia, our expert providers at Specialty Care Clinics will take care of your health and help you recover.
Call (469) 545-9983 to book a telehealth appointment for an at-home check-up.
