WHAT IS CHURG-STRAUSS SYNDROME?
Churg-Strauss syndrome is a disease marked by blood vessel inflammation. This inflammation could restrict blood flow to organs and tissues, sometimes permanently damaging them. This condition is also called eosinophilic granulomatosis with polyangiitis (EGPA).
Asthma is the most frequent sign of Churg-Strauss syndrome. The disorder could also cause other problems, like hay fever, rash, gastrointestinal bleeding, pain, and numbness in your hands and feet.
Churg-Strauss syndrome is uncommon and has no cure. Your doctor or primary care physician could generally help you control symptoms with steroids and other powerful immunosuppressant drugs.
CHURG-STRAUSS SYNDROME SYMPTOMS
Churg-Strauss syndrome differs greatly from person to person. Some people suffer from mild symptoms. Others have serious or life-threatening complications.
Also called eosinophilic granulomatosis with polyangiitis (EGPA), the syndrome tends to happen in three stages and gets progressively worse. Almost everyone with the condition has asthma, chronic sinusitis, and elevated counts of white blood cells known as eosinophils. Asthma generally starts 5 to 9 years before the diagnosis of Churg-Strauss syndrome.
Other signs and symptoms may include:
- Hay fever
- Fever
- Loss of appetite and weight loss
- Joint and muscle pain
- Fatigue
- Cough
- Abdominal pain and gastrointestinal bleeding
- Weakness, fatigue, or a general feeling of being unwell
- Rash or skin sores
- Pain, numbness, and tingling in your hands and feet
- Serious abdominal pain
- Shortness of breath
- Blood in your urine or stools
WHEN SHOULD YOU SEE A DOCTOR?
See your doctor or primary care physician if you develop signs and symptoms like breathing difficulties or a runny nose that does not go away, particularly if it is followed by continuous facial pain. Also, see your doctor or primary care physician if you have asthma or hay fever that unexpectedly worsens.
Churg-Strauss syndrome is uncommon, and it is more likely that these symptoms have some other cause. But it is important that your doctor or primary care physician evaluate them. Early diagnosis and treatment increase the chances of a good outcome.

CHURG-STRAUSS SYNDROME CAUSES
The cause of Churg-Strauss syndrome is widely unknown. It is likely that a combination of genes and environmental factors, like allergens or specific medications, triggers an overactive immune system response. Instead of protecting against invading bacteria and viruses, the immune system targets healthy tissue, resulting in widespread inflammation.
CHURG-STRAUSS SYNDROME RISK FACTORS
Potential risk factors for Churg-Strauss syndrome include:
- Age – On average, people with Churg-Strauss syndrome are diagnosed between 30 years and 50 years of age.
- History of asthma or nasal problems – Most people diagnosed with Churg-Strauss syndrome have a history of serious nasal allergies, chronic sinusitis, or asthma.
CHURG-STRAUSS SYNDROME COMPLICATIONS
Churg-Strauss syndrome could affect many organs, including your lungs, skin, gastrointestinal system, kidneys, muscles, joints, and heart. Without treatment, the disease could be fatal.
Complications, which depend on the organs involved, could include:
- Peripheral nerve damage – Churg-Strauss syndrome could damage the nerves in your hands and feet, leading to numbness, burning, and loss of function.
- Skin scarring – The inflammation could cause sores that could leave scars.
- Heart disease – Heart-associated complications of Churg-Strauss syndrome include swelling of the membrane surrounding your heart, swelling of the muscular layer of your heart wall, heart attack, and heart failure.
- Kidney damage – If Churg-Strauss syndrome affects your kidneys, you could develop glomerulonephritis. This disease hampers your kidneys’ filtering ability, leading to a build-up of waste products in your bloodstream.
CHURG-STRAUSS SYNDROME DIAGNOSIS
No specific test could confirm Churg-Strauss syndrome. Because signs and symptoms are similar to those of other diseases, it could be difficult to diagnose.
The early signs and symptoms, like asthma and sinusitis, tend to be fairly commonplace, so a diagnosis may not be made until the swelling has caused severe damage to organs and nerves.
The 6 criteria
The American College of Rheumatology has established criteria to determine Churg-Strauss syndrome. You are usually considered to have the condition if you have 4 of the 6 criteria. The criteria are:
- Asthma – Most people diagnosed with Churg-Strauss syndrome have chronic, usually serious asthma.
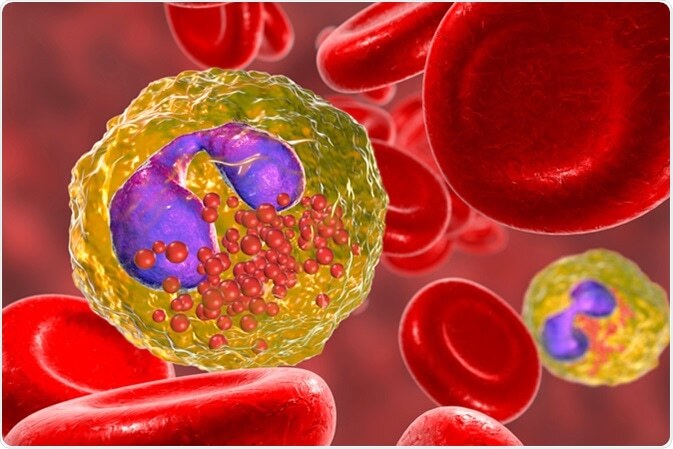
- Higher than normal count of a type of white blood cells known as eosinophils – Eosinophils normally make up one percent to three percent of white blood cells. A count higher than ten percent is considered abnormally high and a strong indicator of Churg-Strauss syndrome.
- Damage to 1 or more nerve groups – Most people with Churg-Strauss syndrome have a kind of nerve damage that causes numbness or pain in their hands and feet.
- Migratory spots or lesions on a chest X-ray – These lesions usually move from one place to another or come and go. Chest X-rays indicate that the lesions mimic pneumonia.
- Sinus problems – A history of acute or chronic sinusitis is frequent in people with Churg-Strauss syndrome.
- White blood cells present outside your blood vessels – Your doctor or primary care physician may order a tissue biopsy of either your skin or a removed nasal polyp to look for eosinophils outside of a blood vessel.
To diagnose Churg-Strauss syndrome, your doctor or primary care physician is likely to request several tests, including:
- Blood tests – When your immune system attacks your body’s own cells, as occurs in Churg-Strauss syndrome, it forms proteins known as autoantibodies. A blood test could detect specific autoantibodies in your blood that could suggest, but not confirm, a diagnosis of Churg-Strauss syndrome. It could also measure the level of eosinophils, however other diseases, including asthma, could increase the number of these cells.
- Imaging tests – X-rays and computed tomography (CT) scans to look for abnormalities in your lungs and sinuses.
- Biopsy of affected tissue – If other tests suggest Churg-Strauss syndrome, you may have a small sample of tissue removed for examination under a microscope. The tissue could come from your lungs or another organ, like skin or muscle, to confirm or rule out the presence of vasculitis.
CHURG-STRAUSS SYNDROME TREATMENT
There is no cure for Churg-Strauss syndrome, also called eosinophilic granulomatosis with polyangiitis (EGPA). But medications could help manage your symptoms.
Medications used to treat Churg-Strauss syndrome include:
- Corticosteroids – Prednisone, which lowers inflammation, is the most commonly prescribed drug for Churg-Strauss syndrome. Your doctor or primary care physician may prescribe a high dose of corticosteroids or a boost in your current dose of corticosteroids to get your symptoms under control quickly. But because high doses of corticosteroids could cause severe side effects, your doctor or primary care physician will decrease the dose slowly until you are taking the smallest amount that will keep your disease under control. Even lower doses taken for extended periods could cause side effects. Side effects of corticosteroids involve bone loss, high blood sugar, weight gain, cataracts, and hard-to-treat infections.
- Other immunosuppressive drugs – For people with mild symptoms, a corticosteroid alone might be enough. Other people need another immunosuppressive drug, like cyclophosphamide, azathioprine (Azasan, Imuran), or methotrexate (Trexall), to further lower the body’s immune reaction. Because these drugs impair your body’s ability to fight infection and could cause other severe side effects, your condition will be closely monitored while you are taking them.
- Immune globulin – Given as a monthly infusion, immune globulin is usually given to people who have not responded to other treatments. The most common side effects are flu-like symptoms that generally last just a day or so. Immune globulin is expensive and does not work for everyone.
- Biologic medications – Drugs like the recently Food and Drug Administration-approved mepolizumab (Nucala), as well as benralizumab (Fasenra) and rituximab (Rituxan), change the immune system’s response and seem to improve symptoms and decrease the number of eosinophils. These medications have been studied only in small trials, and their long-term safety and effectiveness are still not known. Drug therapy could relieve symptoms of Churg-Strauss syndrome and send the disease into remission. But relapses are frequent. Your doctor or primary care physician likely will conduct blood and other tests regularly to monitor your condition and your reaction to the drugs you are taking.
If you or anyone you know is suffering from Churg-Strauss syndrome, our expert providers at Specialty Care Clinics will take care of your health and help you recover.
Call 469-545-9983 to book a telehealth appointment for an at-home check-up.
