DOUBLE UTERUS – SYMPTOMS, CAUSES, AND TREATMENT
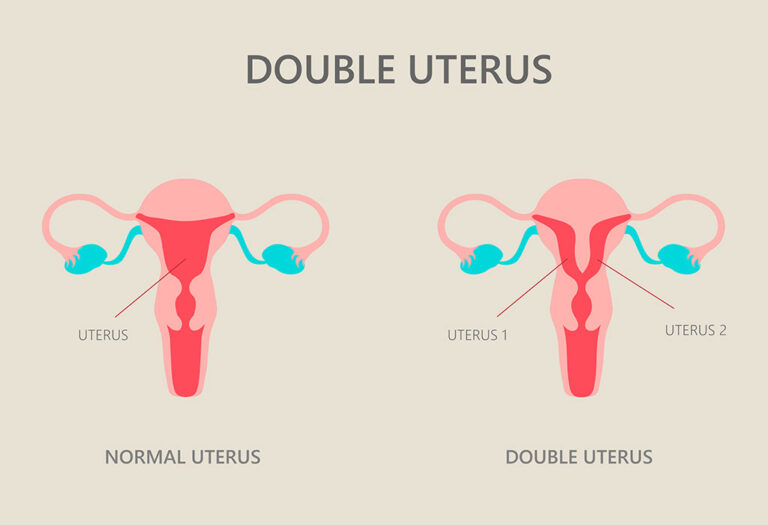
A double uterus is an uncommon congenital abnormality. In a female fetus, the uterus begins with two tiny tubes. As the fetus develops, the tubes normally join together to create one larger, hollow organ — the uterus.
Sometimes, however, the tubes do not join completely. Instead, each one develops within a separate structure. A double uterus might have one opening (cervix) into one vagina, or each uterine cavity might have a cervix. In many cases, a thin wall of tissue runs down the length of the vagina, dividing it into two different openings.
Women who have a double uterus usually have successful pregnancies. But the condition could increase the risk of miscarriage or premature birth.
SYMPTOMS
A double uterus usually causes no symptoms. The condition might be discovered during a regular pelvic examination or during imaging tests to determine the cause of repeated miscarriages.
Women who have a double vagina along with a double uterus might initially consult a doctor for menstrual bleeding that is not stopped by a tampon. In these situations, the woman has placed a tampon in one vagina, but the blood is still escaping from the second uterus and vagina.
WHEN SHOULD YOU SEE A DOCTOR?
Ask for medical advice if you have a menstrual flow despite the insertion of a tampon, or if you have severe pain with menstruation or experience repeated miscarriages.
CAUSES
Doctors are not certain why some fetuses develop a double uterus and others do not. A genetic component might be a factor because this rare condition sometimes runs in families.

COMPLICATIONS
Many women who have a double uterus have normal sex lives, pregnancies, and deliveries. But sometimes a double uterus and other abnormalities of uterine development are related to:
- Infertility
- Miscarriage
- Premature birth
- Kidney problems
DIAGNOSIS
A double uterus might be diagnosed during a routine pelvic examination when your doctor observes a double cervix or feels an abnormally shaped uterus. To confirm the diagnosis, your doctor might recommend one or more of the following tests:
- Ultrasound – This test uses high-frequency sound waves to create pictures of the inside of your body. To capture the images, a device known as a transducer is either pressed against your abdominal skin or inserted into your vagina (transvaginal ultrasound). Both types of ultrasound might be done to get the best view. A 3-D ultrasound might be used where available.
- Sonohysterogram – The sonohysterogram, an ultrasound scan, is done after fluid is administered through a tube into your uterus by way of your vagina and cervix. This enables your doctor to look for problems in the shape of your uterus.
- Magnetic resonance imaging (MRI) – The MRI machine is similar to a tunnel that has both ends open. You lie on a movable table that slides into the opening of the tunnel. This painless procedure uses a magnetic field and radio waves to create cross-sectional pictures of the inside of your body.
- Hysterosalpingography – During hysterosalpingography, a special dye is administered into your uterus through your cervix. As the dye moves through your reproductive organs, X-rays are taken to find out the shape and size of your uterus and whether your fallopian tubes are open.
TREATMENT
If you have a double uterus but you do not have signs or symptoms, treatment is rarely required. Surgery to unite a double uterus is rarely done — although surgery might help you keep a pregnancy if you have a partial division within your uterus and no other medical explanation for a previous pregnancy loss.
If you have a double vagina in addition to a double uterus, you may be a candidate for an operation that would remove the wall of tissue separating the two vaginas. This could make childbirth a little easier.
If you or anyone you know is suffering from Double Uterus, our expert providers at Specialty Care Clinics will take care of your health and help you recover.
Call us on (469) 545-9983 to book an appointment with our specialists.
