WHAT ARE PREMATURE VENTRICULAR CONTRACTIONS?
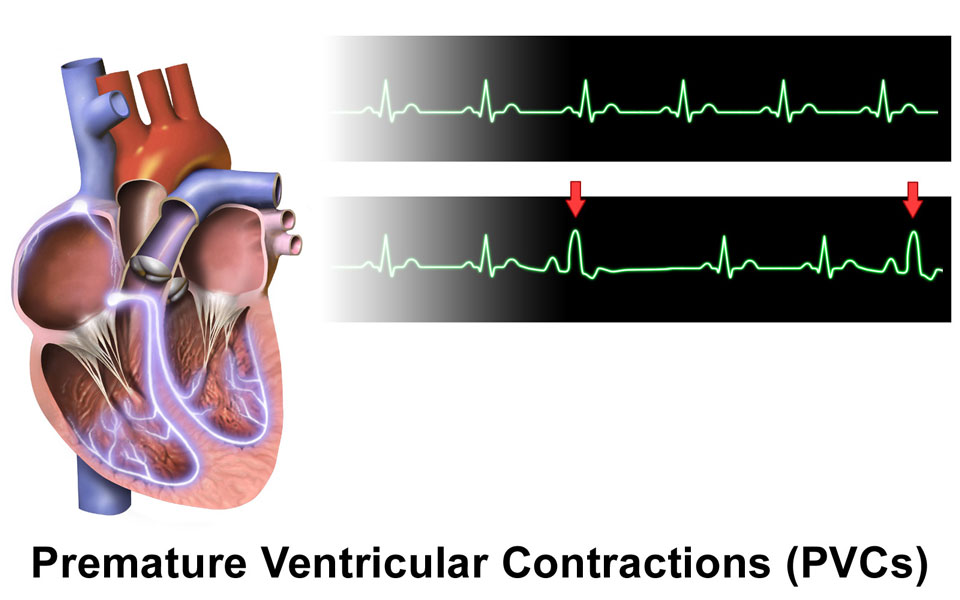
Premature ventricular contractions (PVCs) are additional heartbeats that start in one of your heart’s two lower pumping chambers (ventricles). These extra beats disturb your normal heart rhythm, sometimes causing you to feel a fluttering or a skipped beat in your chest.
Premature ventricular contractions are frequent — they happen in many people. They are also known as:
- Premature ventricular complexes
- Ventricular premature beats
- Ventricular extrasystoles
If you have occasional premature ventricular contractions, but you are otherwise healthy, there is probably no reason to worry and no requirement for treatment. If you have frequent premature ventricular contractions or a hidden heart condition, you might require treatment

SYMPTOMS
Premature ventricular contractions usually cause few or none of the symptoms. But you may feel an unusual sensation in your chest, like:
- Fluttering
- Pounding or jumping
- Skipped beats or missed beats
- Increased awareness of your heartbeat
WHEN SHOULD YOU SEE A DOCTOR?
If you feel fluttering, a sensation of skipped heartbeats, or an unusual feeling in your chest, talk to your doctor. You will want to identify the source of these symptoms, whether it is PVCs, other heart rhythm problems, severe heart problems, anxiety, anemia, or infections.
CAUSES
Your heart is made up of 4 chambers — 2 upper chambers (atria) and 2 lower chambers (ventricles). The heartbeat is generally controlled by the sinoatrial (SA) node — or sinus node — a region of specialized cells in the right atrium.
This natural pacemaker generates the electrical impulses that trigger the normal heartbeat. From the sinus node, electrical impulses pass through the atria to the ventricles, causing them to contract and pump blood into your lungs and body.
PVCs are abnormal contractions that start in the ventricles. These extra contractions generally beat sooner than the next expected normal heartbeat. And they usually interrupt the regular order of pumping, which is the atria first, then the ventricles.
Why do extra beats happen?
The reasons are not always clear. Specific triggers, heart diseases, or changes in the body could make cells in the ventricles electrically unstable. Heart disease or scarring might also cause electrical impulses to be misrouted.
Premature ventricular contractions could be related to:
- Specific medications, including decongestants and antihistamines
- Alcohol or illegal drugs
- Elevated levels of adrenaline in the body that might be caused by caffeine, tobacco, exercise, and anxiety
- Damage to the heart muscle from coronary artery disease, congenital heart disease, high blood pressure, or heart failure
RISK FACTORS
The following could increase your risk of PVCs:
- Caffeine, tobacco, alcohol, and illicit drugs
- Exercise — if you have specific types of PVCs
- High blood pressure (hypertension)
- Anxiety
- Heart disease, involving congenital heart disease, coronary artery disease, heart attack, heart failure, and a weakened heart muscle (cardiomyopathy)
COMPLICATIONS
Having frequent PVCs or specific patterns of them may increase your risk of developing heart rhythm problems (arrhythmias), or weakening of the heart muscle (cardiomyopathy).
Rarely, when followed by heart disease, frequent premature contractions could lead to chaotic, dangerous heart rhythms and possibly unexpected cardiac death.
DIAGNOSIS
An electrocardiogram (ECG) could identify the extra beats and detect the pattern and source.
Electrocardiogram
Depending upon the frequency and timing of your PVCs, different kinds of ECG testing alternatives are available.
- Standard ECG – Sensors (electrodes) are connected to your chest and limbs to create a graphical record of the electrical signals traveling through your heart. This brief test generally is done in a clinic or hospital setting.
If you have infrequent PVCs, they may not be identified during the brief time a normal ECG is being done. In such situations, you may need to use a portable monitoring device for 24 hours or more to capture any abnormal rhythms. Common types of portable ECGs include: - Holter monitor – You carry this device in your pocket or in a pouch on a waistband or shoulder strap. It automatically measures your heart’s activity for 24 or 48 hours, which provides your doctor with an extended look at your heart rhythms.
- Event recorder – This device could be carried in your pocket or worn on a waistband or shoulder strap for home monitoring of your heart’s activity. When you feel symptoms, you press a button, and a brief ECG strip recording is made. The recorder, which could be used for several weeks, enables your doctor to see your heart rhythm at the time of your symptoms.
- Exercise stress ECG – This test uses electrocardiography to measure your heart’s electrical activity while you walk on a treadmill or pedal an exercise bike. It could help determine whether exercise triggers your PVCs.
TREATMENT
For most people, PVCs with an otherwise normal heart would not require treatment. Although, if you have frequent PVCs, your doctor may recommend treatment.
In some cases, if you have heart disease that can lead to more severe rhythm problems, you may require the following:
- Lifestyle changes – Eliminating common PVC triggers — like caffeine or tobacco — could decrease the frequency and severity of your symptoms.
- Medications – Beta-blockers – which are usually used to treat high blood pressure and heart disease — could suppress premature contractions. Other medications, like calcium channel blockers, or anti-arrhythmic drugs, like amiodarone (Pacerone) or flecainide (Tambocor), also may be used if you have ventricular tachycardia or frequent PVCs that interfere with your heart’s function.
- Radiofrequency catheter ablation – For PVCs that do not respond to lifestyle changes or medications, your doctor may suggest ablation therapy. This procedure uses radiofrequency energy to destroy the region of heart tissue that is causing your irregular contractions.
If you or anyone you know is suffering from premature ventricular contractions, our expert providers at Specialty Care Clinics will take care of your health and help you recover.
Call 469-545-9983 to book a telehealth appointment for an at-home check-up.
