WHAT ARE PLANTAR WARTS?
Plantar warts, also known as verrucas, are small growths that generally appear on your feet heels, or other weight-bearing regions. This pressure might also cause plantar warts to grow inward beneath a hard, thick layer of skin also known as a callus.
Plantar warts are caused by human papillomavirus (HPV). The human papillomavirus (HPV) enters your body through small cuts, breaks, or other weak spots on the bottom of your feet.
Most plantar warts are not a serious health concern and generally go away without treatment eventually. You might want to try self-care treatments or see your doctor or primary care physician to have warts removed.
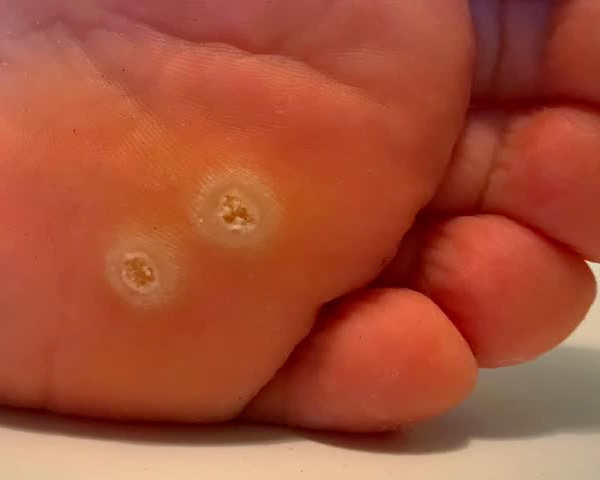
PLANTAR WARTS SYMPTOMS
Plantar wart signs and symptoms include:
- A small, fleshy, rough, grainy growth also called a lesion on the base of your foot, generally the bottom of the toes and forefoot or the heel
- Hard, stiffened skin (callus) over a well-defined “point” on the skin, where a wart has grown inward
- Black pinpoints, which are commonly referred to as wart seeds but are small, clotted blood vessels
- A lesion that intrudes the normal lines and ridges in the skin of your foot
- Pain or soreness when walking or standing
WHEN SHOULD YOU SEE A DOCTOR?
See your doctor or primary care physician for the lesion on your foot if:
- The lesion is bleeding, painful, or changes in aspect or color
- You have tried treating the wart, but it continues, multiplies, or recurs
- Your discomfort intrudes with activities
- You also have diabetes or poor feeling in your feet
- You also have a weakened immune system due to immune-suppressing drugs, HIV/AIDS, or other immune system disorders
- You are unsure whether the lesion is a wart
PLANTAR WARTS CAUSES
Plantar warts are caused by an infection with human papillomavirus (HPV) in the outer layer of skin on the soles of your feet. They develop when the virus enters your body through small cuts, breaks, or other weak spots on the bottoms of your feet.
Human papillomavirus (HPV) is very common, and more than a hundred types of the virus exist. Although, only some of them cause warts on the feet. Other types of human papillomavirus (HPV) are more likely to cause warts on other regions of your skin or mucous membranes.
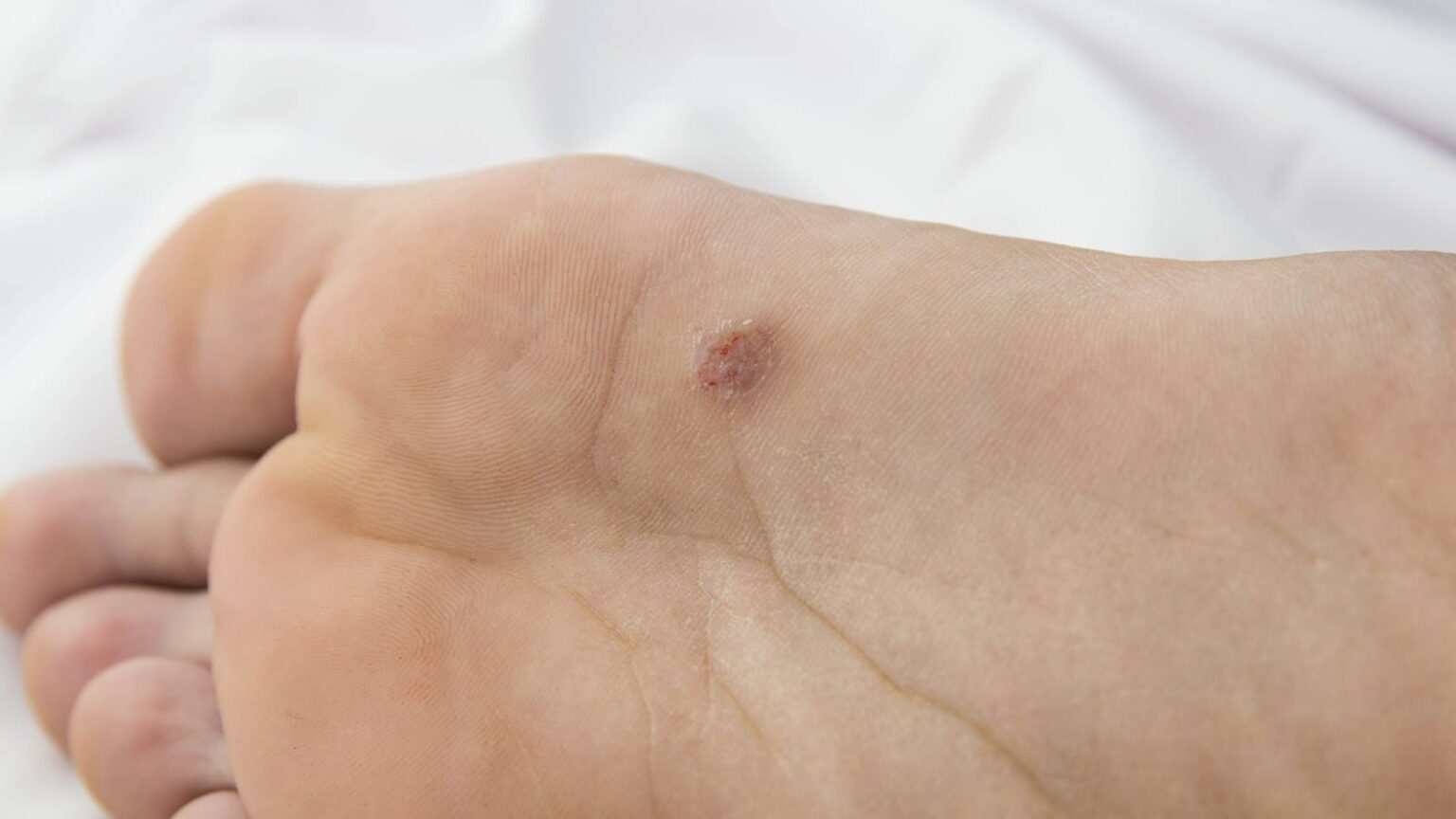
Transmission of the virus
Each person’s immune system responds differently to human papillomavirus (HPV). Not every person who comes in contact with the virus develops warts. Even members of the same family have a different response to the virus.
The human papillomavirus (HPV) strains that cause plantar warts are not highly contagious. So the virus is not easily transmitted by direct contact from one person to another. But it thrives in warm, moist environments. Therefore, you might contract the virus by walking barefoot around swimming pools or locker rooms. If the virus spreads from the first area of infection, more warts might appear.
PLANTAR WARTS RISK FACTORS
Anyone could develop plantar warts, but this kind of wart is more likely to affect:
- Children and teenagers
- People with weakened immune systems
- People who have had plantar warts before
- People who walk barefoot where exposure to a wart-causing virus is common, like locker rooms
PLANTAR WARTS COMPLICATIONS
When plantar warts cause pain, you might change your normal posture or gait perhaps without knowing it. Eventually, this change in how you stand, walk or run could cause muscle or joint discomfort.
PLANTAR WARTS PREVENTION
To lower your risk of plantar warts:
- Circumvent direct contact with warts. This includes your warts. Wash your hands thoroughly once you have touched a wart.
- Keep your feet clean and dry. Change shoes and socks daily.
- Circumvent walking barefoot around swimming pools and locker rooms.
- Do not pick at or scratch warts.
- Do not use the same emery board, pumice stone, or nail clipper on your warts as you use on your healthy skin and nails.
PLANTAR WARTS DIAGNOSIS
In most cases, your doctor or primary care physicians could diagnose a plantar wart with one or more of these techniques:
- Analyzing the lesion
- Paring the lesion with a scalpel and checking for signs of dark, identify dots small clotted blood vessels
- Removing a tiny section of the lesion (shave biopsy) and sending it to a lab for analysis
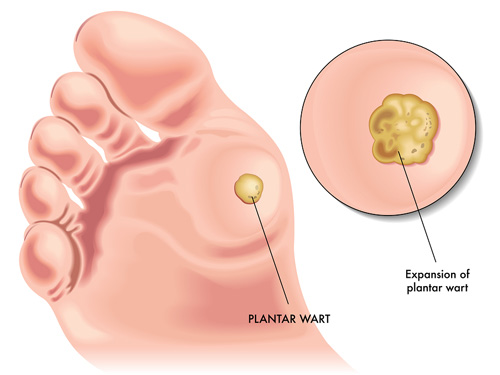
PLANTAR WARTS TREATMENT
Most plantar warts are unharmful and go away without treatment, though it might take a year or two. If your warts are painful or spreading, you might want to try treating them with over-the-counter (non-prescription) medicines or home remedies. You might require many repeated treatments before warts go away, and they might return later.
If your self-care approaches have not helped, talk with your doctor or primary care physician about these treatments:
Stronger peeling medicine (salicylic acid) – Prescription-strength wart medicines with salicylic acid work by eliminating layers of a wart a little bit at a time. They might also stimulate your immune system’s capacity to fight the wart.
Your doctor or primary care physician will likely recommend you apply for the medicine regularly at home, followed by occasional office visits.
Freezing medicine (cryotherapy) – Cryotherapy is done at a doctor’s or primary care physician’s office involves applying liquid nitrogen to the wart, either with a spray or a cotton swab. This method could be painful, so your doctor or primary care physician might numb the area first.
The chemical causes a blister to form around your wart, and the dead tissue splits off within a week or so. Cryotherapy might also stimulate your immune system to combat viral warts. You might require to return to the doctor’s or primary care physician’s office for repeat treatments every 2 to 4 weeks till the wart disappears.
Some studies recommend that cryotherapy combined with salicylic acid treatment is more useful than just cryotherapy, but further study is required.
Surgical or other procedures
If salicylic acid and freezing medicine do not work, your doctor or primary care physician might suggest one or more of the following treatments:
Other acids – Your doctor or primary care physician shaves the surface of the wart and applies trichloroacetic acid with a wooden toothpick. You will require to return to the doctor’s or primary care physician’s office for repeat treatments every week or so. Side effects include burning and stinging. Between visits, you might be asked to apply salicylic acid to the wart.
Immune therapy – This method uses medications or solutions to stimulate your immune system to combat viral warts. Your doctor or primary care physician might inject your warts with a foreign substance (antigen) or apply a solution or cream to warts.
Minor surgery – Your doctor or primary care physician cuts away the wart or destroys it by using an electric syringe (electrodesiccation and curettage). This procedure could be painful, so your doctor or primary care physician will numb your skin first. Because surgery has a risk of scarring, this method generally is not used to treat plantar warts unless other treatments have failed.
Laser treatment – Pulsed-dye laser treatment burns closed (cauterizes) small blood vessels. The infected tissue ultimately dies, and the wart falls off. This method needs repeat treatments every 3 to 4 weeks. The evidence for the effectiveness of this method is limited, and it could cause pain and potentially scarring.
Vaccine – Human papillomavirus (HPV) vaccine has been used with success to treat warts even though this vaccine is not specifically targeted toward the wart virus that causes the majority of plantar warts.
If you or anyone you know is suffering from plantar warts, our expert providers at Specialty Care Clinics will take care of your health and help you recover.
Call 469-545-9983 to book a telehealth appointment for an at-home check-up.
