COMPLEX REGIONAL PAIN SYNDROME
As complex, because it sounds, Complex regional pain syndrome is a simple concept to understand: CRPS may be a pain disorder, usually leading to discomfort and inflammation of the arm or the leg, that one experiences after an injury, stroke, surgery, or attack.
Complex regional pain syndrome may be a neuropathic pain disorder, meaning that it affects one’s nervous system and needs special medical attention
Let us know in detail how to deal with CRPS.
- Incidence of Complex Regional Pain Syndrome in male and female While Complex regional pain syndrome can affect anyone, male, or female, it’s more common for females to be affected by the pain disorder than men.
- Age group affecting Complex Regional Pain Syndrome Similarly, people of any age are often suffering from CRPS, but it’s more common in people between the ages of 20-60 with a peak at the age of 40.
It is known that CRPS is rare in elderly patients and in young children.
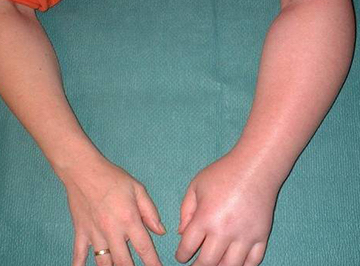
CAUSES OF CRPS
Most CRPS is caused by damaging one’s sensory neurons which successively has secondary effects on the brain. Any trauma on the nerves leads to a deficiency in sending signals to the brain and the affected limb
The most common trauma causing actions or activities are:
- Fractures: Fractures are referred to as one among the common CRPS causes, especially wrist fractures. Dislocation or subluxation of bones must also be taken into consideration
- Sprains/strains: A sprain/strain is defined by an injury that affects the muscles and ligaments of the physical body
- Surgery: CRPS can occur after every surgery, even though it’s successful. Any surgical cuts, retractions, or maybe postoperative scarring can cause Complex regional pain syndrome
- Poor nerve health: Conditions like diabetes, can cause nerves to weaken. The weaker the nerves the harder it’s for them to recuperate after an injury, therefore putting the patients at higher risk of CRPS.
- Minor injuries like Burns and Cuts: Nerve damage is one of the common effects of burn injuries. The severity of the burn depends on the scale of injury of the nerves. Affected nerves are often impaired which leads to incorrect signals to the brain.
- Cuts: on an equivalent wavelength, can also have an impact on the way the nerves work. As they’re very sensitive, any pressure, stretching, or cutting of the nerve may result in the inability to send signals to the brain.
- Limb immobilization: Limb immobilization may lead to compression of nerves making it difficult to move and impaired sensations.
- Poor blood circulation: Impaired blood circulation can affect the nerve signaling in the body leading to CRPS.
- Genetics and environment: Like altogether medical cases, genetics and therefore the environment plays a serious role in recovery. Within the case of CRPS, genetics also because the environment the patient grew up in, influences the speed and therefore the ability to get over an injury, therefore putting the patient more or less in danger of developing Complex regional pain syndrome.
HOW DO I KNOW IF I AM SUFFERING FROM CRPS?
These are the symptoms that seem to work out if you’ve got CRPS:
- Swelling of the affected/ painful area,
- Changes in skin temperature. a continuing change between hot and cold feeling skin.
- Changes in complexion, varying from red and blue to while and blotchy skin.
- Changes in skin texture.
- Changes in sweat production. A patient with CRPS may feel that their skin is excessively sweaty.
- Affected areas may develop hypersensitivity to the touch or cold
- Affected areas may leave you with a continuing throbbing pain or burning sensation.
- Changes in hair and nail growth. which will be experienced as rapid hair growth or no hair growth in the least
- Increase in muscle spasms, and weakness of the muscles
- Decreased ability to maneuver the affected part
Like with every medical condition, it’s important to notice that symptoms vary from person to person and not everyone experiences the same symptoms. The symptoms that one may experience can vary depending on time also.
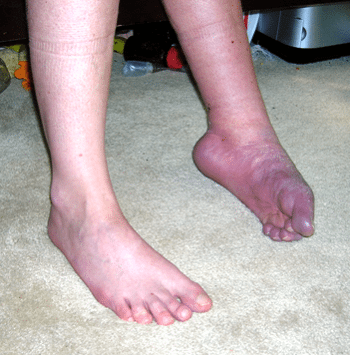
THE THUMB RULE TO KNOW THE SYMPTOMS OF CRPS
As mentioned above, while everyone has different experiences, there’s a general rule of thumb.
- Pain
- Redness
- Swelling of the affected area
- Changes in hypersensitivity
Skin temperature is usually the symptom that you simply might experience first. With time, comes the following symptoms
- Paleness
- Cold sensation of the affected limb
- Skin and nail changes
- Muscle spasms
- Tightening
Once any of the changes occur, they’re now irreversible.
DIAGNOSING CRPS
- Once you’ve experienced any of the symptoms and confirming or denying the likelihood of being suffering from CRPS is on your mind, here are a number of the points for diagnoses that will allow you to know CPRS
- No specific test will determine if one has CRPS, but a radical examination by a neurologist, orthopedist, or maybe a cosmetic surgeon (anyone who has any familiarity with nerve anatomy) is a method to diagnose
- Getting an MRI, CT scan or ultrasound will help image the nerves and also detect any abnormalities within the bone marrow or the affected area.
- A triple-phase bone scan will help localize and diagnose CRPS by determining if the breakdown and absorption of bone tissue are abnormal in any area of the body.
SEE YOUR DOCTOR IMMEDIATELY TO GET TREATED WITH CRPS
It is best if CRPS is detected and treated early. Therefore, if one experiences constant, insufferable pain in any of the limbs also leading to severe inability to touch or move an equivalent limb, a diagnosis by a medical professional is best.
Treatment for CRPS
The good news is that for early and mild cases of CRPS, no treatment is required because it will recover on its own.
In the circumstance where treatment is required, here are a number of the first therapies used:
- Medications: The medications usually used are Non-steroidal anti-inflammatory drugs, local anesthetic ointments also as Opioids
- Psychotherapy: A side effect of any disorder is the psychological state of the patient. So, it’s important for the patient to undergo psychotherapy so as to stop them from not seeking medical aid or engaging in their rehabilitation. If longer time passes without treating CRPS, the brain functions and activity will worsen.
- Graded motor imagery: GMI may be a therapy that consists of convincing the patient’s brain that the pain is not any longer there. By simply imagining moving a painful part of your body, pain-free, your brain is going to be tricked into not creating pain. Patients will check out a mirror and visualize themselves moving the affected part without actually moving it.
- Medulla spinalis stimulation: Stimulating electrodes into the medulla spinalis will send tingling sensations to the affected area, which can help block pain sensations and instead normalize sending signaling into the medulla spinalis and brain
REDUCING PAIN AND RE-ESTABLISHING CIRCULATION FOR CRPS
If you’re experiencing mild CRPS, reducing limb swelling and re-establishing circulation is usually the key to activating recovery. These are some tips to follow to regulate CRPS flares:
- Rest and meditate
- Stretch and obtain massages
- Distract yourself from the pain
- Elevate affected limbs while sleeping to assist excess fluid to return to your heart
- Exercise daily to enhance blood circulation
- Try compression socks or sleeves which can help limit swelling.
CAN I DO ANYTHING TO STOP CRPS?
After experiencing an injury, the road to recovery is the next milestone. Follow these steps to stop CRPS while on the road to recovery:
- Consume vitamin C regularly to avoid inflammation
- Get on your feet and out of bed. After a stroke, it’s important to start mobilization early.
- Consult a physiotherapist.
- The sooner you “treat” the newly recovered limb the less likely you’re to develop CRPS. Physiotherapy and Rehabilitation will help improve blood flow and stop circulatory symptoms, also maintain flexibility, strength, and rework the affected limb to its original function.
If you or anyone you know is suffering from unexpected spasms and pain with redness & inflammation all over your body, you may have CRPS (Complex Regional Pain Syndrome).
Call us on (469) 545-9983 to book an appointment with our pain management specialists.
